Public Health, the Francis Report and Mid Staffordshire Hospital
Am I alone in being a bit surprised how quiet the public health world is about Mid  Staffordshire Hospital NHS FT and the Francis report?
Staffordshire Hospital NHS FT and the Francis report?
I am not sure if this comparative silence is because Directors of Public Health have little responsibility here (see the Department of Health guidance for local government on the role of Directors of Public – Best Practice Guidance – issued in December 2012), or whether the profession is just breathing a collective sigh of relief because it is not under the media spotlight.
I think that public health has a crucial role to play here. Reading the Francis report I am clear about two things
- First – there was a culture of disrespect and appalling treatment to vulnerable people who expected the health service to care for them at a time when they were in great need.
- Second – that because of this treatment it is the case that some people died because this lack of care. However, it is unclear how many people did actually die. The report which is full of caveats and doubts presents a debate which walks around a figure of something between 400 to 1200 people over a period of 12 years. In other words between 33 and 100 people a year from April 1996 to March 2008 (Mid Staffordshire NHS FT Inquiry Vol 1 Section G Mortality Statistics Page 350 onwards). I really hope that I have understood this correctly – please feel free to correct me.
I do not want to diminish the awful experiences of people who had the misfortune ot be ‘cared for’ at Mid Staffs Hospital – but I am concerned that this focus on a poorly performing hospital and the next five that are in the pipeline diverts us from much wider failures in care and public health.
What concerns me is that there are much more significant examples of system failure – with a much greater incidence of preventable death and yet we accept them – there is no Francis Report to challenge these.
At a recent LGA Public Health Conference the excellent Chris Bentley gave a presentation on “Health and Wellbeing Boards with teeth – Interventions that Bite” . One of the challenges for Health and Wellbeing Boards is having a proper grip on the balance between need and actions to address these.
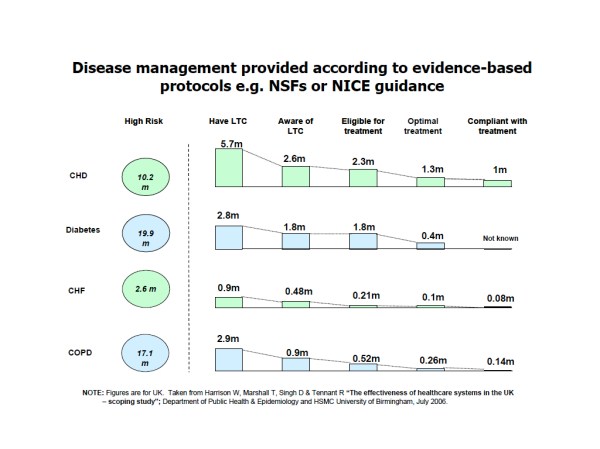
In his presentation he shared information from a study conducted by the University of Birmingham in 2006. The slide is below. We can see that in the UK there were 5.7m people who had CHD of whom the health system (I read this as primary care) was aware of only half and of these only 50% were compliant with their treatment. So of the total population of people with CHD only 20% were actually receiving and taking the treatment they needed! This is system failure on a massive scale – not in hospitals but in primary care in particular.
Of course it is worse than this – because there is a strong inequalities gradient to this picture and as Chris would be the first to say there is an even wider issue to do with societal inequalities such as poor quality housing, low income and lack of power.
As local authorities start to develop their leadership role with regard to the Health and Wellbeing of their communities it will be crucial that they take a balanced response to the challenges presented by Francis. This will mean a measured and thoughtful view on where the real system deficits are in their area and which are the ones that it is important to focus on. This view will affect the focus they place on relationships with the provider trusts, what they hope Healthwatch will achieve and most importantly the level of scrutiny they give to primary care provision and to work to address the social determinants of health.
It will be crucial that local public health provides a thoughtful and confident analysis that allows local politicians to get this balance right – otherwise we will end up being led by high profile, government led, media fuelled reports about priorities and not address much greater injustices locally.
I share your concern:
“What concerns me is that there are much more significant examples of system failure – with a much greater incidence of preventable death and yet we accept them – there is no Francis Report to challenge these.”