Transforming Participation in Health and Care – what should Clinical Commissioning Groups do?
 NHS England are currently coming to the end of a consultation on a guide titled Transforming Participation in Health and Care. Its always risky to have titles like this – because stakeholders then look to them with raised expectations. Sometimes I think it might be better to go for titles such as “Improving things little by little – participation in health care” or “Steady as she goes – some ideas about improving things a bit in participation in health care”!
NHS England are currently coming to the end of a consultation on a guide titled Transforming Participation in Health and Care. Its always risky to have titles like this – because stakeholders then look to them with raised expectations. Sometimes I think it might be better to go for titles such as “Improving things little by little – participation in health care” or “Steady as she goes – some ideas about improving things a bit in participation in health care”!
I am not going to comment on the document directly. Here instead are five areas that I thought about when I read the document – some of these are mentioned in the draft guidance others are not or are not mentioned strongly enough.
Role of Clinical Commissioning Groups.
The old NHS paradigm sometimes felt like it was based purely on how each commissioning or service improvement process involves the public. While this is important if we are to genuinely transform participation in health care CCGs also need to provide place leadership in partnership with local authorities to shape how the local health and wellbeing system involves the public.
Unlike provider organisations CCGs have this system level responsibility.
So, this cannot just be about involving the public in individual commissioning processes that CCGs manage. It has to be about CCGs sharing responsibility for how an area (local authority level) provides ways for citizens to participate in the local health and wellbeing system.
Clinical Commissioning Groups therefore need to work with providers to ensure that they have powerful systematic actions for ongoing public involvement. In particular as a member of Health and Wellbeing Boards CCGs need to ensure that the participation of the public occurs across service AND organisational silos.
CCGs must also promote (with local authorities) a shared approach to driving forward good practice and building local capability. This should include explicit strategies to:
- Build local capability and capacity at a system level – to enable citizens (particularly from disadvantaged communities) to build on their interest in their health and wellbeing and that of their families and communities so that they can confidently get involved.
- bring joint investment to key local infrastructure organisations
- ensure explicit approaches to working across services and organisations to share practice and information and report on these to the health and wellbeing board.
- Championing dialogue and challenge across provider organisations
Effective Models of Participation by the Public in Commissioning.
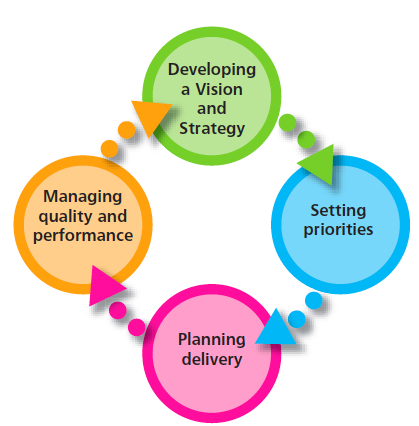
Many of the models of Commissioning that are promoted by the NHS tend to be neat and tidy – for example the old World Class Commissioning Model – this graphic is taken from the Patient and Public Engagement Toolkit – South Central:
These flow charts reflect how commissioners imagine the world to be not how it actually works – they are led by how finances are organised; financial year reporting requirements; 3 year funding programmes; target delivery requirements and election cycles. They do not reflect how we live our lives as citizens and what we need in order to engage and influence.
We need models that start from how the public experience the world not how the system feels the world should be. For example I do not manage my personal relationships on the basis of some conceptual model of needs assessment, analysis, commissioning, review and recommissioning. Of course those of you who know me might argue that I would benefit from this!
So, CCGs will need to recognise that developing relationships with people in order to increase accountability and strengthen co-production actually requires approaches that foster stability, consistency and the long term. They need to provide flexible, long term points of entry built on trusted relationships – such as those developed by neighbourhood organisations like development trusts and healthy living centres.
So I think that a public centred model for participation might look a bit like this:
Active relationships with an empowered public
Powerful relationships with the public require commissioners to take a balanced approach to investing in support – this means taking a shared responsibility with local government in particular for the relationships that people have with sectors and institutions. It is crucial therefore to share responsibility for commissioning key local institutions such as Adult Education, Voluntary Sector Infrastructure Organisations – such as those that support volunteering and generic and specialist community development organisations – particularly those that operate at a neighbourhood level.
It also means recognising that it is important to foster mechanisms that promote dialogue and challenge. I am actually not convinced that we should have a core target that 80% of stakeholders should be feeling satisfied with regard to how CCGs have involved people. Dissatisfaction and disagreement are powerful drivers for positive change – promoting targets that call for high degrees of satisfaction feels really dangerous to me – not least because as Ibsen tells us “the majority is always wrong”!
Knowing what is going on
Clinical Commissioning Groups must work through Health and Wellbeing Boards to establish agreed ways of testing whether the level of public participation and involvement is adequate. I think that Health and Wellbeing Boards with active support of the CCGs should be commissioning intelligence reviews that capture the level and type of engagement that is happening within the health system so that providers and commissioners can be held to account for the degree involvement and participation.
Lets face it we could all benefit from a continuing evidence based dialogue to help us build on good practice and tackle areas of weakness. Frankly if Francis tells us anything at all it should be that we need to establish mechanisms locally that stop us deluding ourselves that we are ‘good’ at participation.
Volunteers
I do think that any guidance on participation has to recognise the key role of volunteers. These are people who are actively involved in co-production. Either through delivering services or helping to develop or manage them. I think that there is a strong relationship between the number and quality of volunteers and the effectiveness of work to increase participation.
What do you think?

Thanks Mark for another thought piece!
A few thoughts came to mind when reading this:
Language – in your opening paragraph, agree that this is a critical feature when establishing a dialogue – e.g participation. In what? for what reason? maybe getting involved in…could be more accessible?
At what level are organisations needing and wanting people to be involved/participate (and vice versa) – in their health? health management/maintenance? Organisational change? I’m not sure the CCG positions are particularly nuanced or sophisticated enough on this. I agree with your point on the 80% satisfaction type statement too. It’s crass.
“We need models that start from how the public experience the world not how the system feels the world should be….” to achieve any progress on this a CCG and/or LA would need to be very radical and dispense with the business as usual paradigms on involvement/participation and invest resources with people/groups that can develop more sensitive and fluid models and approaches – relational difference, power, collaborative, mediated…on behalf of the organisation and communities, with local people. It’s not really rocket science in terms of what’s known to be helpful in terms participatory process and methods – can CCGs be radical and brave in such ways, really shift the emphasis and relational focus? After all, if we look at social media platforms (Twitter for example) there are lots of people very active and participating in the (local and national ) health debate – but maybe not directly with the organisation(s) or system managers – how can such people come together and seek a new advantage through collaboration on an issue? Maybe its healthy for people to be on the outside of the tent as protagonists?
More later perhaps…
This is interesting, but I do not understand how your diagram would work. It does put the individual at the centre, which makes sense, but how does a big, complex, corporate entity like the CCG have a relationship with that model? What does it look like?
Our local population are not at all ’empowered’. The level of dialogue is , ‘I cannot get an appointment at the doctors’ or ‘they were all lovely when I got my hip done’. I am part of the CCG ‘participation’ group- we are trying to support people to be able to look at things strategically- while also paying attention to the concerns as they are expressed just now.
Truly, though, I don’t know how to take a valued citizens view of the world, and develop consensus, and agree contracts, all in the challenging timescales we work to. What would have to happen to make a start? Maybe strengthen the 3rd sector.
Thanks Ruth – a perfectly fair challenge! Here are some quick thoughts on some of the headings in my diagram:
“the information and skills I need” Once a CCG starts to ask questions about where does a member of the public get the skills and information they need to engage that leads commissioners to look at investing in information and training that addresses this. So – some places invest in community health champion programmes like Altogether Better or in Turning Points Community Researchers or in Expert Patient Programmes.
“Make a contribution” If a CCG starts to ask questions about how do they value peoples voluntary contributions to health and care it leads to the development of actions that are about capturing the scale of the contribution of volunteers, consideration of which areas have lots of volunteering and which do not, assessment of how people are supported and trained as volunteers etc.
“Share my experience and opinions” What are the routes and processes that are available to the public to be heard – which ones are formal, which ones are about accountability, which ones are ongoing – there are a huge and growing range of methodologies here (Patient Opinion, NHS Choices, Complaints, Friends and Family etc etc) – they have different purposes and reach – we need to be clear which ones a CCG should expect to have in place as a minimum.
Bear in mind of course that I am not claiming to have the answers here! I am just sharing my thoughts and ideas – contributing to the debate.
Oh yes – and I agree completely with your last comment – invest in the third sector!
Best wishes – Mark
Very helpful. Thanks.
I am a contributor to the NHS England guidance to commissioners- which is where your piece notionally started, I believe. I am fully aware of how feeble CCGs are in this area, but I am hopeful that the guidance might gently nudge in the right direction.
The challenge is to put measurables and ‘must do’s in, to create culture change. Hearts and minds versus ticky boxes. I know that without some boxes to tick, some CCGs will not change at all, but focussing on the measureables is not the outcome we really want.
Answers on a postcard, please.
Very interesting. In my experience, those closest to understanding patient involvement acknowledge their limited viewpoint, and start with a theme, or service, or portion of care pathway they wish to get to know more deeply. Once they have some focus, they also need to be led by those who have experience in it. I prefer semi structured interviews to questionnaires, I prefer open space to focus groups, because sometimes you need to take time out to hear what people really want to tell you, not what you think they want to talk about. My view is that community champions make excellent trusted intermediaries for this activity.
Liz
This is a really important discussion, and its also a very live one. Think some of the change will come if CCGs start to see the benefits that investing in volunteers can bring.
If they can see that training and developing Patient Leaders and Quality Improvement coworkers, will help them make that case for change, and for withdrawing funding from hospital care in order to invest in prevention or self care , then it will really help them.
CCGs will be facing bad press or criticism locally as they reduce services, and if they learn to work with service users, the VCS and Healthwatch, to do this in ways which are coproduced, they will really benefit.
I mean this literally. They should pay to train up say a dozen volunteers as Patient Leaders and learn skills to take them from using their own experiences , to advocating for patients generally. They should also start to work on Quality Improvement, using tools like Plan, Do, Study Act PDSA cycles to learn from what has gone right and what has gone wrong , in the last commissioning cycle, or the last Board meeting.
And totally agree that Community Champions can often critique and improve any plan or commissioning intention and improve it.
Nicola
Reblogged this on thepositivevoice.
Reblogged this on HUMAN RIGHTS & THE SIEGE OF BRITAIN POLITICAL JOURNAL.