The welfare benefit system is a public health system

This blog is based on a talk I gave at the recent Faculty of Public Health Conference – reacting to the Ken Loach film I Daniel Blake.
In a recent blog I set out how public health has struggled to recognise the important contribution that the benefits system makes to wellbeing and tackling health inequalities. We need to think of the benefit system as a public health service.
Nonetheless, we are in a position where this crucially important Public Health Service is increasingly difficult to access and where it is even hard to have a discussion at a local level about how we can ensure that vulnerable populations make best use of it.
A reminder – the NHS budget is just over £100 billion a year and the social welfare spend is £126 billion – not including pensions.
In fact as the figure below from Simon Duffy (Centre for Welfare Reform) shows the actual cost of social welfare to the state is considerably less than this.
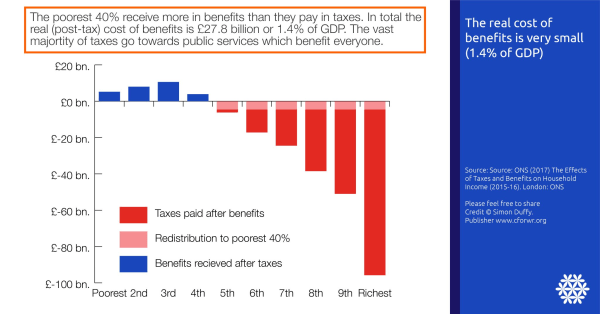
When it comes to public health strategies and practice at a national level we look to two agencies to scope the landscape – Public Heath England and NICE. Between them they would argue that they describe the strategic public health challenges and actions needed to improve population health and tackle health inequalities.
At the conference we heard that this is not the case. Both agencies work within the constraints of Government Policy – Public Heath England strategic focus has to be consistent with the government agenda – not only does it not publicly challenge DWP actions – the only time it mentions welfare payments in its strategies is with regard to actions that will reduce their take up! It also does not offer strategies and actions to ensure that the benefit system is used to its best effect.

NICE works to a shopping list of priorities signed off by Government – again this list does not include welfare benefits.
This means that we must not accept that the Public Health England Strategy includes all the issues we need to address and the actions we can take or that it even includes the most important ones! In fact the Public Health England strategy is based on a mixture of evidence and a government ideology.
Local Action
Luckily, local Public Health teams have a degree of autonomy from central government. However there are challenges here too. It is quite difficult to have a system level conversation about access to the welfare benefit system – I think that this is for three reasons:
- Poisoned Minds – Local leaders find it difficult to engage with an issue that has been represented by large elements of the press and respective governments as being about scroungers and layabouts.
- Pot of gold – Partly for the reason above local decision makers would rather focus on creating employment and getting people off benefits which is of course commendable. However, there are many unable to work, low paid jobs rely on benefit top up and there is some evidence that people with good financial security through appropriate welfare support are likely to find employment more quickly than those ‘incentivised’ through punitive benefit regimes.
- Welfare Economy – I suspect that some local leaders worry that a focus on improving access to the benefit system will lead to accusations that they lack ambition and are building an economy that is dependent on ‘handouts’.
Actions
Five actions for local Public Health.
- Narrative and Conversation – have a strategic conversation at an appropriate level which considers what is known about need, levels of financial insecurity and demand on benefits services (this is difficult because DWP release little local data). Data sources could include StepChange, Citizens Advice, Insolvency Judgement trends, Public Health funeral (Paupers Funeral) trends, local Food Bank data etc. Organisations like the Centre for Welfare Reform and the Money and Mental Health Policy Unit can offer analysis.
- Investment – consider the current level of investment in welfare rights services – what stories do providers tell of the strategic picture? Too often their data is kept at contract manager level in local systems rather than being used to develop strategies.
- Focus – Often local Citizens Advice Services are left to get on with it – there is plenty of demand out there. Local commissioners need to understand the whole population effect – in particular are services targeted on the most vulnerable? For example:
- People with mental health problems such as those receiving IAPT or on the Care Programme Approach
- People with progressive long term conditions such as Cancer – Macmillan has done tremendous work here
- Families in poverty especially those who are expecting new children
- Collaboration – Local Public Heath teams can help by pulling together welfare rights providers and NHS provider and commissioners to consider how to strengthen the contribution of welfare benefits to people with long term conditions.
- Evidence – local Citizens Advice services have a long track record of translating issues faced by their clients into evidence to challenge policy (I gave a Sheffield example here) local Public Health Teams need to consider how they can strengthen this.
What do you think?
You have hit the nail on the head. Excellent summary of welfare rights as the great untapped resource & missing link in the public health system. Refreshing that you have highlighted local leaders reluctance to talk about it or take action to include welfare rights as a fundamental foundation & building block for public health. Are you aware of any papers on this theme covering Scotland? Thank you
Thanks for your comments Katrina – they are appreciated. I’m afraid that I am not aware of any papers that apply to the Scottish experience – it would be interesting to know if Harry Burns or the Glasgow Deep End group have done any work on this?
I will have a word with Simon Duffy from the Centre for Welfare Reform he may know – if he does I will add to this comment – or someone else may spot this and respond!
Best wishes – Mark
Great blog as ever.
There’s something about systematically unpacking the complexity that underlies “the determinants of health”. From the outside the Heath care system may look like a big homogenous blob of doctors and nurses. From the inside it is not. Similarly “the determinants of health” are a series of systems, each belie vast complexity.
There’s no doubt that the “welfare system” is a determinant. And that changes to it over recent years have had profound detrimental impacts on our mental and maybe physical health, at population and individual level.
Making meaningful intervention in this space requires DEEP understanding of the system to be able to carry credibility and authority and thus to be able to effectively influence.
One might say the same of “housing”, of “education”, of “early years”, or of “planning”. And so on.
Each of theses systems is vastly diverse and complex with many different cultures and sub cultures. Many different, difficult and odd incentives with people pulling in many different directions.
As a jobbing DPH, I cant be, and am not, expert in all areas. I know a bit about some of them. Definitely, an effort is needed to shift balance of “public health” away from “health” as defined as health care services. Most know my view that “health
NHS) and that “lifestlyes” might be better characterised as commercial determinants of health
(As an aside there’s an interesting conundrum there. Should we ignore “smoking” because it is a downstream lifestlye issue, and result of “choices individuals make”…. It causes c12% of illness and 20% of death.)
Also I know you’ve given PHE a hard time for being too physical health centric and lifestyle centric….maybe it’s good to expand the range of actors that are involved in the pursuit of “public health” – knowingly or unknowingly, even if those actors don’t call it public health, doesn’t really matter to me if the objective is shared. To be fair it’s my type that need to play into this agenda rather than vice versa
Certainly in Sheffield we are clear that PH = organisational responsibility and not a “department” or a line in the budget. This is easier said than done, there’s an element of (my) “personal” responsibility and accountability.
But yes, “welfare” is a definitive public health system. Public health types (defined narrowly and with a big P and a big H haven’t engaged in it as well as we might. Let’s put that right?
Cheers Greg – and welcome to the blog! I agree with you – we have a range of social support systems and others like education that are about personal development and change – yet most of them are tremendously complicated to access for individuals and hard to understand for many professionals.
When we met recently I flagged up that I have had a green flag to establish a special interest group on this topic within the Faculty of Public Health and am very keen that we extend an invitation to a number of welfare system experts to work with us – so watch this space.
Yes, I have given PHE a bit of a hard time – but only because their role is so important -their position and expertise represents the biggest single chunk of Public Health resource for change in the country it therefore needs to be relevant!
All the best – Mark
Hi Mark – I really like this blog and have been making this point in various places. Hope you don’t mind – I was planning on using your sketch above in a talk on health inequalities to the socialist health association – I have referred them back to this blog. Thanks Ben
Hi Ben pleased you like the blog and the illustration – of course you can use it! All the best – Mark