The NHS Long Term Plan and Social Prescribing

While welcomed in some quarters the NHS Long Term Plan has come in for a fair amount of criticism for its lack of strategic heft and poor focus on the relationship that the NHS must have with external partners such as local government and the voluntary and community sector.
One of the areas where it does recognise the importance of making connections between communities, their assets and the voluntary sector is with regard to Social Prescribing.
Social Prescribing has developed a fair amount of traction in the NHS. Indeed, the term itself speaks to front line health professionals such GPs, it uses their language and it has gathered around it some significant champions such as Dr Michael Dixon who was also the founding Chair of the NHS Alliance.
This is what the NHS Long Term Plan says:
I think this means that by 2023/4 900,000 people a year will be offered Social Prescribing by the NHS. Note the commitment to 1,000 social prescribing link workers. I have allocated them by population size of CCG so for example Sheffield get 10 and Corby 1 (my full CCG list is here) of course doing it this way takes no account of inequality. The statement about NHS Social Prescribing Link workers has generated anxiety in the voluntary sector who are the main providers currently – with concern that these will be NHS employees.
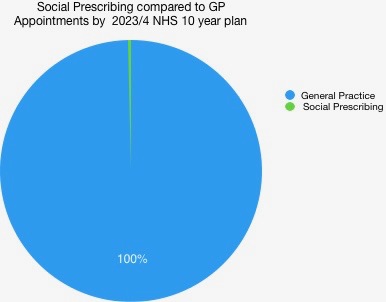
At the moment there are about 59.7 million patients registered with GPs who make over 240 million appointments a year. compared to the 900,000 a year promised for Social Prescribing. This means that in 5 years time social prescribing activity will be equivalent to .38% of appointments at GPs. Here is an illustration of the scale of this.
If you are an average patient and see your GP four times a year the odds of you being offered a Social Prescribing appointment are approximately once in every 60 years!
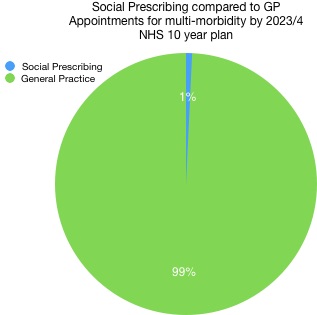
Of course it is fairer to say that not everyone who sees a GP will need or want referral to social prescribing. It is probably more realistic to focus on people with multi morbidity. A recent study by the Department of Public Health and Primary Care at the University of Cambridge showed that over half of GP consultations are now with patients with multi-morbidity – this equates to 120m appointments a year.
The pie chart below shows how the NHS England social prescribing commitment would impact on this challenge. It is clear that the current NHSE commitment still gets nowhere near – indeed it could be said that the NHSE response is so diluted and small that it will be almost homeopathic in terms of its system level effect!
Real scale of the challenge
I mentioned in an earlier blog on Welfare Rights and Health that a joint paper produced by Citizens Advice and the Royal College of General Practice estimated that approximately 20% of GP time was spent with patients who presented with non clinical issues that would be better addressed elsewhere.
I think that this proportion is likely to be much greater with when General Practice is providing a service to disadvantaged communities who are likely to have to higher levels of multi-morbidity and a greater level of non clinical issues.
Finally there is a subsidiary point even a small target of just under a million people receiving social prescribing services will have a knock on effect to voluntary sector services. Some existing social prescribing services such as Rotherham have a degree of funding that recognises this. The NHSE 10 year plan does not seem to recognise this.
What this means
The current ambition set out in the Long Term Plan leaves social prescribing as a bit of a sideshow for the next 5 years. There is a real risk that once the magical 900,000 a year target is met that the foot comes off the gas – with little having been achieved.
- Maybe this level of ambition matches need?
- Perhaps only 1% of people who see GPs require social prescribing?
- If it is only a minority interest then should more thought be given to ensure that this investment is reaching out to those who would benefit most rather than being generally available?
- Given the small scale of investment are there other interventions such as Local Area Coordination, Community Development and Health Trainers that might have a greater impact that should be considered by NHS England too?
What do you think?

Mark, are you in danger of taking this “Long Term Plan” too seriously? Am I being too cynical in thinking the current Tory party, obsessed by Brexit and still committed to “austerity” and the steady dismantling of public provision and its replacement with private arrangements, has any other intention than kicking this complex and “wicked” question into the long grass?
Ha! Loved your comment Mike – it made me laugh – which is frankly welcome these days! Have to keep plugging on though – I hope that my audience is not primarily NHS England – more people on the ground who are trying to do something meaningful in the current policy context – hope all is good with you. Mark
At least, there is some commitment to social prescribing within the long-term plan however pathetic it might be. I suppose the danger might be that CCGs take the number estimates as being what they should be providing rather than a minimum.
Thanks Nigel – I agree positive that there is some commitment there – it opens a door to discourse and negotiation at a local level……hopefully! Best Mark
Great article Mark, excellent presentation of the actual facts, I wonder who at NHSE thought this through before making such bold statements in the plan. I am a passionate advocate of SP but despair at this being showcased as something new! It may well have a recognisable label these days but anyone who has worked at community level in recent decades will scream from the hilltops with frustration. That said, I am still pleased to see it on the agenda and supported by Sir Michael Dixon and HRH Prince of Wales who attended the first SP conference held at the Kings Fund a couple of years ago. Until 2015, I worked at a national level within the NHS. Previously I was a CEO in the voluntary sector in Cheshire. My first role in the NHS was to undertake a review of all voluntary sector spending across central and eastern Cheshire. I collaborated with the local authorities in Cheshire at the time and the review revealed that between the PCT and the LA we were investing just on £6m a year in the sector but not telling anyone about the services. I banged on many a GPs door asking them to refer patients into the services the PCT and LA commissioned, alas to no avail. However, the goal posts have moved significantly since with some excellent models of SP working across the country, all have involved additional investment, with one in Halton (funded by Halton CCG) seeing a Care Coordinator from Wellbeing Enterprises sat at the MDT meetings within GP practices when a decision is taken to refer into the service. Whilst the medical model of health is to be acknowledged, respected and applauded, it is not always the answer a patient seeks. A person-centred approach to health reaps the greatest rewards. The conversation on SP is still in its infancy because without equal funding to support comprehensive role-out i fear it will become just another tick box exercise.
Thanks for your contribution Hilda – really interesting – I agree with you – I think one of the big issues is a tendency by NHSE and local commissioners generally towards solutions that offer an attractive simplicity and that once in place become examples that appear regularly in annual reports as indications that they are being taken seriously ….. but comparatively little has changed on the ground. All the best Mark
I think it is important that social prescribing should not just become the latest flavour of the month and cause a loss of focus on good work already done by local authorities and the voluntary and community sector as well as wider engagement through programmes like MECC. We should be aiming to weave social prescribing into existing programmes and structures so that it genuinely adds value. I also have a professional interest in asking whether the new link workers will be regulated in any way.
Good to hear from you David – yes I agree re weaving in to wider engagement programmes. It is clear that while it is to be welcomed that greater connection with communities is seen as important there is real concern at a local level that a one size fits all model from the top will weaken local activity. Interesting point re regulation of link workers – and given your role not surprising! I think there is a need for a discussion here – there are lots of roles that are concerned with helping people access and navigate complex systems that are not regulated such as PALs and Welfare Rights Workers, Health Trainers – that is not to say that training and managerial structures to ensure competence are not important – but I am not so sure about regulation – best Mark
Excellent, thanks Mark. I’ve drawn attention to this locally (not sure it’s being seen as a leading issue in the Plan). About 2/3 of practices in Gateshead, where I worked last year, have some form of SP paid for by the practice, so for many the idea and value is not under debate, and I know many Health Care workers in Primary Care are working to resolve social issues, rather than working on purely ‘medical’ ones. I think it’s a bit naive to assume there is capacity within communities/Third Sector for activities to refer into – in more deprived areas in particular the prevalence of knitting groups and ballroom dancing sessions may be lower (!) and it’s likely this sort of referral will not resolve more complex issues (debt, social isolation, low level mental health issues). The challenge of approaching health more holistically and having a number of tools available depending on what that person needs (drugs, hospital, social contact, money to live on) continues.
Norma! Lovely to hear from you – spot on – its good that connection with communities is recognised in the NHS Long Term Plan but we do need a more sophisticated approach that recognises complexity, diversity and disadvantage – all the best Mark
Hi Mark,
Although I broadly agree with the point that the current funding for social prescribing is unrelated to need, I am not convinced that your analysis of consultation rates is accurate. You are saying that ‘social prescribing activity will be equivalent to 0.38% of appointments at GPs’. You derive the figure by (900,000/240m)*100=0.38%. Doesn’t this calculation assume that each of the 900,000 people meet their GP once a year? This does not seem to account for the fact that most people who are supported by social prescribing are frequent attenders to their GP. So for example, social prescribing users in City and Hackney go to see their GPs eight times a year (median). If you calculate that over one year, 900,000*8= 7,200,000 so the impact would be more like 3% which looks very different from 0.38%, although perhaps still low. So perhaps your broad point is still valid but the magnitude is different.
Currently, there is a significant disproportion between the NHS target of 900,000 and the number of people who need support. For example, there are about 15m people experiencing long term conditions (King’s Fund data*) and the number 900,000 refers to a ‘universal’ social prescribing scheme which is therefore offered to anybody, not just people on long term conditions. See the Universal Personalised Care document for more details. https://www.england.nhs.uk/publication/universal-personalised-care-implementing-the-comprehensive-model/
I also agree with your point about the proportion of people with social issues (rather than just clinical) being higher than 20%, in disadvantaged areas. It would be good to see a study that spells this out properly.
And again, I agree with your point about Rotherham which is often talked about but much less imitated as it requires CCGs to fund VCSE delivery of support services. There are indeed other systems to fund this, for example, social impact bonds in Ways to Wellness (Newcastle) or community prescribing in Newham which followed an approach based on payment by result. All of these have advantages and disadvantages but I thought I would flag it up.
Finally, I am worried about the funding for social prescribing going to Primary Care Networks which may decide to do their own things rather than build on what’s already there and, once again, reinventing the wheel. I hope I am wrong
(*) https://www.kingsfund.org.uk/projects/time-think-differently/trends-disease-and-disability-long-term-conditions-multi-morbidity
Thanks Marcello – first, apologies for being so slow approving your comment – I thought I had done this. second, I take your point about my maths but I am not saying that there is a relationship between social prescribing and general practice (although I am sure there is), I am just comparing the scale of GP appointments versus the number of people seen for a ‘social prescription’ I acknowledge this is crude – but my point is to question whether the scale of investment and ambition is actually at the right level – which I know you go on to say too. I agree completely with your final point – this is a live concern to community anchor organisations where I live in Sheffield. Best wishes Mark