What on earth is going on? Data, Health Inequalities and Localism.
I was in a local authority meeting recently and someone said – “the problem with keeping track of the impact of the economic crisis on the poor is that we don’t have the resources to do it!”.
keeping track of the impact of the economic crisis on the poor is that we don’t have the resources to do it!”.
This meeting was part of a piece of work I am doing for the Institute of Health Equity who have been commissioned by the London Health Inequalities Network to develop a set of indicators that will help London Boroughs map the impact of the economic crisis and the government policy response on health inequalities.
The starting point was to undertake a literature search to establish which factors have the greatest impact on health inequalities. The outcome of this work which was led by Ellen Bloomer was a good report “The impact of the economic downturn and policy changes on health inequalities in London” This found that the following determinants have a substantial impact on health inequalities:
- Unemployment – unemployed individuals particularly the long term unemployed have a higher risk of poor physical and mental health compared with those in employment.
- Income – Living in poverty is associated with worse mental health outcomes, particulalry among women.
- Housing – Both with regard to access to housing and its quality.
- Mental Health – one of the outcomes that is affected by all of the above determinants is a greater likelood of poor mental health.
The next step was to start to pull together the indicator set based around these determinants. This work is still ongoing and I am not going to talk about it directly. One of the challenges that has emerged is that many of the official indicators that are used by statutory agencies are not that helpful when it comes to mapping real time impacts on the most excluded populations. I think that this is for a number of reasons that include:
- Not gathered frequently enough to usefully inform yearly commissioning cycles
- Tend to capture service demand rather than actual circumstances of people in need
I also suspect that a number of existing data sets assume that things like economic crises don’t happen and that government policies won’t try to substantially redefine who is deserving and underserving. Both these assumptions are clearly mistaken.
To reiterate – I think the key issue is capturing peoples actual circumstances and to avoid being confounded by measures of service useage or definitions of deserving and undeserving that change according to policy whim.
The data is out there.
I am increasingly confident that the data does exist but it is currently not easily accessible to local commissioners. I think it sits in 3 places. National Government, the third sector and the private sector.
National Government
The Department for Work and Pensions (DWP) clearly has information on every individual who is currently claiming benefits. However much of this information is not easily available at borough level or on a sufficiently frequent basis to enable local authorities to have an accurate picture of what is happening within their populations. There are obviously problems with this data. It is after all a rationed service and populations can ‘disappear’ if need is redefined to exclude people.
Third Sector
A number of voluntary organisations have access to useful data. One of the best is Consumer Credit Counselling Service whose 2012 report documents the shocking rise in clients with pay day loans, the impact on people who rent and the growth in need for debt advice among older people.
At the moment none of this (very good) information is available at local authority level or more frequently than yearly. In case you think that CCCS is a small voluntary organisation – in 2011 they supported 370,000 people – there are approximately 23 million households in the UK at the moment – so CCCS is supporting more than 1% of UK households every year!
There is also useful data held by services like Citizens Advice who have received some development funding from the Department of Health to help them develop their information systems to provide information at local authority level for Joint Strategic Needs Assessments.
However, the reality is that much voluntary sector data – even that held by big nationals is not easily accessible often because intelligence gathering systems lack the capability to provide the information in useable form to help commissioners.
There is of course a growing recognition that the personal narratives and experiences of people that are often captured by voluntary and community organisations are in themselves a powerful source of intelligence.
Private Sector
The best data is of course held by the private sector. It is interesting that the the Department of Health has focused on ways to try to persuade the private sector to make the services they provide healthier (Department of Health Responsibility Deal) rather than seeking to persuade private sector agencies to share what is potentially a much greater asset – their data.
In my view the most powerful private sector data source is CAIS (Credit Account Information Sharing), this is run by Experian and holds information on most of the adult population – 440 million credit accounts of which 33 million are currently in default.
The type of information that CAIS holds on each credit account includes:
- The lender
- The borrower, e.g. full name, full address
- Type of account (loan, mortgage, etc.)
- Default date
- Current balance outstanding
- Repayment amount and term
- Credit limit
- History of payment over the last 36 months
All of this information is available to be shared across all member agencies. Membership is managed through the Steering Committee on Reciprocity which is a cross industry forum made up of pretty well everyone you could think of:
- British Bankers Association
- British Retail Consortium
- Consumer Credit Association
- Council of Mortgage Lenders
- Credit Services Association
- Energy Retail Assocation
- Finance and Leasing Association
- Mobile Phone Operators
- UK Cards Assocation
So…….the data is there and systems are in place to share it already.
What the Department of Health needs to do.
As a key advocate for localism the Department of Health needs to create the environment where this will flourish. Local Commissioning needs data that is relevant to place and supports Health and Wellbeing boards drive forward cross sectoral strategies to address health inequalities.
The Department of Health needs to:
- Persuade key players within the private sector – starting with the financial institutions – to share the data they hold with local government
- Invest in a systematic programme to support the third sector to modernise its intelligence analysis capability.
- Ensure that that other Government Departments starting with DWP provide the data they hold in a form that can be used by local authorities.
Health Inequalities – Kings Fund critiques Department of Health and offers actions for Joint Health & Wellbeing Strategies.
The Kings Fund report ‘Clustering of Unhealthy Behaviours over time’ builds on evidence from the Health Survey of England to present some useful ideas and actions on tackling health inequalities at a local and national level.
The report is essential reading for all local health leads – because of its critique of government policy and the actions that it proposes. It will help in the development of local Joint Health and Wellbeing Strategies.
In summary it says that:
- The overall proportion of the population that engages in 3 or 4 unhealthy behaviours has declined significantly from 33% of the population in 2003 to 25% by 2008.
- However, these reductions have been seen mainly among those in higher socio-economic and educational groups.
- People with no qualifications were more than 5 times as likely as those with higher education to engage in all 4 poor behaviours in 2008 compared with only 3 times as likely in 2003.
One of the dangers of a focus on healthy behaviours is that the policy priority becomes one of blaming the most disadvantaged and focussing on changing their behaviours rather than helping people change their socio-economic circumstances.
As the report acknowledges (page 17):
“our choice of lifestyles – and the cut-off points for what is termed ‘unhealthy’ behaviour are obviously subjective”
AND
“we do not know whether the effectiveness of strategies to change behaviour differs according to the comparative ease of change”
“how do large changes in income or wealth, moving in or out of employment .. impact on taking up multiple behaviours or reducing them?”
Behaviours as a way in to socio-economic issues.
Starting with behaviours always makes me feel uncomfortable – because I am clear that it is people’s socio-economic circumstances that are the biggest determinant of wellbeing. and Duncan Selbie the Chief Executive designate of Public Health England agrees – stating that the balance of factors that impact on wellness are:
- social and economic – education, employment, and violent crime, 40 per cent
- health behaviours – alcohol, tobacco and sexual behaviour, 30 per cent
- clinical – quality and access to health care, 20 per cent
- environmental – air and water quality and building design, 10 per cent
Nonetheless the report provides a useful way into this wider agenda and uses the population behaviour data to argue for a more coherent system level approach to addressing health inequalities.
It builds on a couple of useful reports. The first is a Department of Health one – “Healthy Foundations – A segmentation model” which provides a helpful framework to make the case to commissioners for a model that is built around active citizens.
Grit your teeth if you don’t like being put in a box.
The Healthy Foundations model has two elements:
3 overaching dimensions collectively determine peoples ability to live healthily:
- Age/Life Stage
- Circumstances/Environments
- Attitudes/Beliefs towards health and health issues
It then identifies 4 further sub-segments that describe different ways we respond to our circumstances.
- Fighters – people living in negative environments who are standing above the norms and have a high level of motivation to look after their health (in the States they would be called Positive Deviants).
- Thrivers – people living in positive environments who have a high level of motivation in looking after their health.
- Survivors – people living in negative environments and who have a low level of motivation in looking after their health.
- Disengaged – people living in positive environments who for some reason have a low level of motivation in looking after their health.
The model is useful – because it recognises the importance of the circumstances we live in and the need to challenge cultural norms and it is simple enough for commissioners to understand. It provides a framework around which we can have a debate about where the balance of investment should be. Of course we need to argue that the definition of ‘Fighters’ encompasses activists who are championing greater citizen control for their communities.
The Kings Fund report makes a number of recommendations for action.
It starts off by providing conditional support for “Every Contact Counts” (p19) the governments soundbite policy on health improvement. While it calls for investment in training and support for staff to implement it presents a more thoughtful and nuanced view than that promoted by the Department and its Strategic Health Authorities. Noting that “successful intervention is likely to require coaching and structured decision making support to help people with multiple risk factors to focus on areas that motivate them and give them the confidence to change”.
This does not sound like “every contact counts” at all noting that “people are likely to require a more long term relationship rather than a series of one off interventions” it suggests that the policy would be better titled ‘every relationship counts’. This feels better particularly when combined with its next recommendation “Exploiting the potential of lay and peer support” (p20) recognising that “lay and peer support offers considerable potential for tackling multiple lifestyle risks… which offer tailored advice, motivation and practical support to people wanting to adopt healthier lifestyles delivered by staff who are representative of their communities”.
The report notes that “appropriately skilled health trainers and lay ‘health champions’ represent an under-used and ready made workforce to help drive the reduction of multiple lifestyle risks in the context of local joint health and wellbeing strategies. This role has a good fit with the ‘Fighter’ group described in the Healthy Foundations document mentioned earlier.
Local Wellness Systems
Finally, the report recognises the importance of system level approaches at a local level. A counterpoint to the failure of Government to offer joined up policies. It highlights the excellent briefing ‘From illness to wellness’ produced by the NHS Confederation in association with the Faculty of Public Health. Drawing attention to the integrated wellness service model – which provides a good basis for Joint Health and WellBeing Strategies.
Conclusion
This report and the links it makes provides a helpful addition to the toolkit for local champions who are arguing for a coherent system level focus on inequalities that places a greater emphasis on closer relationships with citizens.
Do you remember Strategic Health Authorities? Most people were completely unaware of their existence and they had no accountability to local people. Yet they were the key mechanism used to shape the priorities of Primary Care Trusts – when the Strategic Health Authority blew its whistle all PCT managers stood to attention. The NHS Commissioning Board is their new incarnation – “it will oversee the way that over £80bn of taxpayers money is spent to secure NHS services in England”. So in the world of localism how does the draft Mandate for the NHS Commissioning Board help us tackle inequalities and increase citizen control?
The Department of Health consultation on the mandate closes on the 26th of September 2012
There is a great deal in this document – which feels more grounded and relevant for local activists than the NHS constitution. The NHS Commissioning Board will pull the strings of Clinical Commissioning Groups and commissions GPs so the mandate will be crucial in terms of setting the tone locally.
Local citizens and organisations will need to be clear about the ambition within the mandate in order to encourage and challenge Clinical Commissioning Groups and to motivate Health and Wellbeing Boards to challenge or ignore the NHS CB on areas where it is weak or passively implementing poor government policy.
Overview
I am going to look at the following sections:
- Section 2 Improving our Health and our Health Care – which focusses on 3 main areas – Inequalities, Mental Health and Health Improvement.
- Section 3 Putting Patients First
- Section 4 Broader Role of NHS
Section 1 – Improving our Health and our Health Care
Inequalities
Strengths – Clear and Strong Statements
- tackling inequalities “a central priority for the Board”
- “Its about inequalities in access and outcomes”
- “Board must focus on those attributable to social deprivation as well.”
- “The Government expects the Board as far as possible to make progress towards reducing inequalities across all NHS Outcomes Framework Indicators”
- “the NHS cannot achieve world class health outcomes for all without a particular focus on those who are disadvantaged, vulnerable or socially excluded”
Weaknesses – Only commits to setting inequalities outcomes for Domain 1 (preventing people from dying prematurely) of the NHS Outcome framework initially. Leaving those for enhancing quality of life for people with long term conditions; helping people to recover from episodes of ill health or following recovery; ensuring people have a positive experience of care; and treating and caring for people in a safe environment for a later unspecified date.
After 2 years The Governments Inclusion Health Programme is getting referenced in policy documents but has not produced any work of significance & has no public profile – the only public document is an archived one produced by the last government.
Implications for local champions – Clear statement provides plenty of opportunity to create a coherent argument at a local level. However, CCGs will need to be encouraged to take a broader approach where no explicit outcome measures exist – this will be challenging.
With no mention in the mandate of the social determinants of health or co-production of services with citizens local champions will need to develop assertive local models to push CCGs to establish strong links with agencies tackling the Social Determinants of Health & co-production with citizens.
Mental Health
Strengths – Strong Statement to put Mental Health on a par with physical health.
Key document is Mental Health Implementation Framework which is a powerful cross government plan produced with a range of statutory and voluntary sector partners.
Weaknesses – It is unclear what national leadership the NHSCB will be expected to provide with regard to making connections with other key national agencies and in championing this agenda across other government departments.
Implications for local champions – CCGS will need to be pushed to have approaches that include focus on social determinants such as access to welfare rights – when the NHSCB will be promoting a narrower agenda.
NHSCB representatives will need to be held to account by local champions through Health and WellBeing Boards with regard to actions they are taking at a national level to promote this agenda across government.
Section 2 – Improving Health
Strengths – “NHS has a vital role in improving the publics health through helping us stay healthy”
Weaknesses – Feels incoherent and lacking in strategic impact – mixture of traditional service roles – Screening, Immunisation and Health Visitors and weak internally focussed plans such as improving the health of the NHS workforce and sound bite ideas such ‘Every Contact Counts’
Implications for Local Champions – CCGs will need to be encouraged to take a broader and more coherent approach than the NHSCB. They will need to be encouraged to engage critically with poorly thought through ideas such as ‘Every Contact Counts’.
Section 3 – Putting Patients First
Strengths
- “Patients as joint participants in their own care and recovery”
- Recognition of role of carers
Weaknesses – No description of how the NHSCB will ensure strong public engagement in its own work or accountability to local areas.
- Focus on the individual as driver for change – personal budgets and choice.
- Emphasis on Information Strategy – which is very IT based
- Proposed drivers – ‘choice and personalisation’ not proven as main drivers for improving quality.
- Hard to see how the NHSCB will support local efforts to develop new delivery models like health champions
Implications for local action – persuading CCGs that there are valid roles for active citizens who are involved in improving roles of their own health, their families and communities. Ensuring that the collective action and long term relationships with communities is understood and developed.
Section 4 – Broader Role of NHS
Strengths – Recognition that NHS needs to work more in partnership with other sectors and agencies – for example improving childrens chances of achieving as good eduction responsibility of health services as well as local government and schools
Need to prevent hard to reach groups “falling through gaps”
Weaknesses
- There is a strange shopping list of priority areas that feel like they have been put together on the back of an envelope – Children and Young People, Crime, the Armed Forces and promoting growth, innovation and research.
- The NHSCB comes across as part of Government. We get no feeling that this will behave any more independently than Strategic Health Authorities – a passive government delivery structure with no mind of its own – unlike local government.
- No recognition of the role of the voluntary and community sector
- No clear responsibility for supporting and funding capability and innovation within primary care and CCGs.
Implications for local action – Need to build alliances with local government and CCG to develop more coherent strategies for addressing need that are a counterweight to the narrow list imposed on the NHS CB.
What do you think?
Are Private Companies better at providing Healthwatch?
The answer is yes if you are in Lancashire, Greenwich, Lewisham, Harrow and Essex and Southend Councils. They all have contracts with Parkwood Healthcare to provide LINks or in the case of Lancashire County Council – Healthwatch.
In their blogs Paul Cotterill and David Floyd have already questioned whether letting Healthwatch contracts to the private sector is consistent with the requirements of the Health and Social Care Act.
I want to use the Parkwood experience to illustrate some of the issues arising from the increased marketisation of the public and voluntary sectors.
Parkwood Holdings
Parkwood Health Care is part of Parkwood Holdings PLC who are the second largest private sector operator providing management services for local authority sports, recreation, education and cultural services. According to their annual report for 2011 they employ over 5,000 staff (almost 3,000 FTE) and have an annual turnover of £114m.
Parkwood Holdings consists of 4 divisions – Parkwood Leisure (managing local authority leisure services), Glendale (horticulture and estate management), Parkwood Consultancy Services and Parkwood Health Care.
Parkwood Healthcare which had a turnover of £1.9 million in 2011 ‘is a medical services business based on a nursing agency but also includes facilitation work withiin the community based on the LINks programme’.
In 2009 they decided to “refocus on the ‘healthy living’ agenda adopted by the NHS.” (Annual Report 2009 page 14)
In addition to the LINk contracts it runs a nursing agency business – with branches in Central London, Manchester and Bishops Stortford this had a turnover of £1m. It also provided Health Trainer services in Buckinghamshire, Berkshire West and Leicester and South East Essex .
In their 2009 annual report (page 15) Parkwood say:
“Parkwood Healthcare’s role is to act as a host for voluntary organisations to meet and influence service provision. In this respect these contracts have a research and consultancy element.
Parkwood Healthcare has also submitted bids for obesity management contracts, advocacy programmes and counselling services. Parkwood Healthcare would like to establish a full medical and clinical bias to this market, but must first gain sufficient credibility with a full range of simpler largely non-medical contracts, to penetrate this market.”
I interpret this to mean that initiatives like LINk/Healthwatch are helpful because they allow Parkwood to develop a greater understanding of the market.
Conflict of interest
The Care Quality Commission are not allowed to set up and run health services. However, at a local level it does seem that some commissioners consider it acceptable for the same organisation to run front line services and at the same time to be responsible for scrutinising all local health and care services.
For example Parkwood clearly have ambitions to expand into a range of front line health services and they are also in the business of running LINk/Healthwatch services that scrutinise locally commissioned health services – some of these may be their competitors and others might be provided by Parkwood – in Essex Parkwood already provide both the health trainer service and the LINk.
I am not suggesting that Parkwood have behaved unethically – but I do feel that potential conflicts of interest needs to be addressed in a clear and transparent way – this is primarily the responsibility of commissioners.
I think that there are a number of voluntary organisations that may also be in this position too – providing local services and delivering the LINk – however in most cases they will not have the ability to make such a strong impact across the market place as a large private sector company and they will therefore be less able to use the intelligence and profile they might gain through Healthwatch as a foundation to build other services from.
Holistic Approach
Interestingly the Parkwood model – with its strong leisure services and environment portfolio puts it in a very good place to compete as a public health provider. Parkwood in partnership with Bristol City Councily recently opened the PFI £27m Hengrove Park Leisure Centre which include a Health Living Zone where provides a range of services including screening, smoking cessation and nutrition.
As I noted at the beginning leisure service provision is one of Parkwoods main business areas – they are clearly seeking to build out from here to offer a more inclusive health and wellbeing offer.
Voluntary Sector
LINk services involve volunteers – until now the voluntary and community sector has considered it to be one of its unique selling points. I would like to understand what volunteers working for a LINk/Healthwatch which is run by a private sector company feel about how their contribution is being used to contribute to that companies market position and profits.
Conclusion
Parkwood are clearly a successful and innovative organisation with considerable credibility with a number of local authorities. In addition to this they seem to have a good understanding of the market opportunities that are available to them and a business model that is arguably more in tune with current policy and practice than some public health departments!
What I have tried to show is the implications that the current policy context and the approach of local authority commissioners has for the voluntary sector – particularly with regard to Healthwatch – in summary:
Citizens
- There are occasions when Healthwatch (as with LINks) will need to launch campaigns to challenge commissioners or providers. How can we ensure that such campaigns are not weakened because the organisation providing Healthwatch is also a potential provider in the market affected by the campaign?
Local Commissioners
- I am not convinced local commissioners are sufficiently clear about how to ensure that Healthwatch providers have no potential conflict of interest when it comes to bringing challenge and scrutiny to local health systems. Both with regard to whether a Healthwatch provider is already provider health services and where they may be scrutinising potential rival providers.
Voluntary Sector
- It cannot be assumed that local commissioners understand the added value that key specialist organisations like Councils of Voluntary Service or Citizens Advice Bx bring. They are generally not in the market for broader health and social care contracts but are instead focussed on their core offer around infrastructure support or welfare rights and advocacy.
- Volunteers – I think there are some broad issues for the voluntary sector to consider about the implications of volunteers working for private sector providers.
Scale
- While the quality of each of the LINk websites run by Parkwood and their outputs does vary a bit – it is also clear that they have benefited from some of the strategic and analytical expertise that Parkwood Healthcare can offer. The Voluntary and Community Sector need to learn from this and consider how – collectively and through collaborations – it can respond and compete.
Public Health
- There are clearly lessons to be learned from private sector providers who are seeking to develop a coherent approach to responding to the health and wellbeing challenge – and are also interested in partnerships from other sectors.
If you have not read ‘the Power of Information’ – don’t. At least not until you have read the the Equality Analysis first – this is excellent – it gives a succinct summary of the strategy and follows this up with a well researched description of the challenges we face with regard to accessing and using health information.
It is no coincidence that the Equality Analysis has been co-produced with the support of a range of voluntary and user led organisations (page 20)
The ‘Power of Information’ is a response (para 1.3) to the consultation on Liberating the NHS: An Information Revolution and to the Information report produced by the NHS Future Forum. As the NHS Future Forum states (para 5.4):
“…..information technology is only part of the story about data sharing, and not the main part (my emphasis). Time and again it was put to us that the effectiveness with which information is shared is primarily a matter of culture and behaviour”
The strategy goes on to devote almost 90 pages to promoting a technical solution to information sharing – using information technology.
Of the 30 plus case studies in the strategy I reckon that 85% are concerned with IT led interventions – the majority of which are concerned with data sharing between professionals. This highlights the real challenge.
There are already plenty of examples of IT data storage projects out there. But far fewer examples of projects that describe ways in which information can be shared systematically directly between people – professionals and patients – and even fewer that do not involve IT. The failure of the strategy to address this is one of its significant deficits.
The strategy is concerned with using information technology to:
- give all people access to their health records
- share information about individuals between health systems
- keep track of utilisation of services and interventions
- publish a more comprehensive and accessible range of performance and outcome data
What the Equality Analysis says:
- 9.2 million adults have never accessed the internet
- Those aged 65+ are much more likely to be offline than younger people – 60% of adults aged 65+ have never accessed the internet. Of the almost 17 million finished consultant episodes of people staying in hospital in 2010 the largest group (21.7%) were adults between the age of 60 to 74
- Only 15% of people living in deprived areas used online government services in 2009
- 40% of the UK population do not use online channels, including websites such as DirectGov and NHS Choices – see for example research conducted by the University of Bedforshire in 2010
- The average reading age of the UK population is 9 years.
- There is a risk that already excluded groups such as people with learning disabilities, gypsies and travellers will not benefit from access to health and care inforamation such as medical records to the same degree as the rest of the population.
- ‘a lack of primary care data in relation to ethnicity means we have no systematic data available for ethnic health inequalities’ (page 14)
In addition to deficits and challenges the Equalty Analysis also makes a strong case for positive solutions – particularly through those provided by collaborations with the voluntary and community sector.
“There is evidence from the Voluntary and Community Sector that partnershps between specialist VCS groups and GPs, Trusts and clinics help to improve patient understanding, choice, use and access to information and therefore the patient ability to manage conditions and make effective decisions. There is an opportunity to improve information sharing with these groups by encouraging commissioners of health and care services to work with community led and user-owned organisations, to reach people in ways they can engage with.”
This is followed by positive examples with regard to HIV and work with blind BME women. (pages 13/14)
Equality and the Power of Information
There are sections in the strategy that recognise the above issues. For example among the 90 pages there are two paragaphs which state:
- “we want information to benefit everyone and reduce (not increase0 health inequalities – with appropriate support for the many of us who need it in understanding and using information effectively – in particular we are clear that not being able to acces the internet should not be a barrier to information.” (para 4.1)
- “…the aim is for everyone to benefit ….this will mean that some of us will need extra support to use information as a core part of our care services” (para 4.15)
Unfortunately the above paragraphs are about as much detail as we get in the main strategy. Instead it devotes the rest of the document to detailed descriptions of universal IT led solutions.
It fails to sufficiently recognise the very specific and significant exclusions identified in the Equality Analysis and to propose in sufficient detail the actions that will be required to address them. It does not appear to have taken into account the Institute of Health Equities work on proportionate universalism.
There is a real risk – at a time of austerity – of further disenfranchising some of the most easily ignored and vulnerable communities; diverting energies to create a universalist model when we need to focus on bringing already discriminated groups up to the same level as the rest of us.
Key Issues
- Inequalities – I restate this because it is so important – an information strategy that does not prioritise work on excluded communities is a failed strategy and will worsen the inverse care law.
- Social Determinants of Health – I know that data sharing between health and social care is important but the document does not do enough to reach out to other sectors – housing, environment, employment etc. This will is perpetuate a siloed approach to health and wellbeing. There is a vague commitment to addressing this issue in the ‘long term’ in paragraph 5.52 – Local authorities and CCGs are grappling with these issues now!
- Voluntary and Community Sector The focus of the strategy is on data in the statutory sector – NHS and Social Care – there is a real danger that of excluding the voluntary and community sector here – and of also not giving sufficient value to the strong relationship offer that the sector brings.
- Relationships – As the Equality Impact Assessment makes clear ‘the power of information’ is not just about individuals accessing their personal records, or having their prescriptions bar coded – its also about the relationships they develop with each other, their carers, professionals and other services. The starting point has to be service responses to specific need – by all means work to a set of principles around data sharing – but it is responses to people with needs in the circumstances that they live that matters.
What do you think?
My last post focussed on the importance of local leaders driving needs  assessments and commissioning through using commissions to ask the tricky and difficult strategic questions that systems need to address.
assessments and commissioning through using commissions to ask the tricky and difficult strategic questions that systems need to address.
I want to focus on another example of effective commissioning to address the Social Determinants of Health – this time from an organisation which has its roots in clinical support to people with cancer – Macmillan Cancer Support.
One of the challenges in tackling the social determinants of health is in convincing local commissioners that a particular service or intervention is worth investing in.
The response from commissioners – particularly in the NHS – is usually something like “show us the evidence that this works and we will consider investing in it”. This response, particularly in these straightened times is usually sufficient to send us scuttling away to our burrows – to try to address the often impossible task of demonstrating the causual link between a social determinant, health outcomes and savings to the NHS……….we rarely re-emerge.
Those of us who have been involved in this field know that once we hit the social determinants of health – out in the real world – it is really hard to identify the causal relationship between a social determinant of health and its specific impact on populations in a way that satisifies a local commissioner – this is because outcomes are often long term and multi-factoral.
I think that one of the reasons that we face this problem is because of the divide between commissioning and provision that successive governments have promoted over the years. This has been driven by:
- an attempt to bring greater scrutiny and accountability into how public funding is used.
- a concern that providers cannot be trusted to make decisions that are always in the best interests of the public – this has become a bigger issue as services have become privatised and therefore cannot always be assumed to working in the public interest.
The key point is that the driver for the commissioner/provider split is not actually ensuring quality of provision – it is instead a rather poor attempt at ensuring accountability for how public money is spent.
The purchaser/provider split means that commissioners have had to increasingly rely on proxies for experience – quantitative data and evidence generated through research – to help them make decisions. This is because the needs of the public and their experience of service delivery is not something that commissioners are directly exposed to. This is of course one of the reasons that is given by the Department of Health for the creation of CCGs – GPs will be both providers and commissioners of services.
The lived experience of people with Long Term Conditions
Arguably the biggest challenge that the NHS faces is how best to respond to the needs of people with Long Term Conditions – 2/3 of the NHS budget is spent on this area (Patient Involvement and Public Accountability NHS Future Forum p3).
So I was interested to read an article recently in the Guardian written by Jan Morgan who had experienced a severe stroke. What is striking about this powerful and moving story is how her quality of life and wellbeing was most affected by her access (or lack of access) to the financial support that she was entitled to. Her difficulties in getting this support had a huge impact on her recovery and wellbeing – and hence on her utilisation of NHS services.
One of the key services that helps people with Long Term Conditions navigate the complex and off-putting government social welfare system are welfare rights services.
Yet it remains very hard to convince the Department of Health and the NHS of their central importance for the reasons that I have explained at the beginning – the response is still too often – show us the evidence!
Macmillan Cancer Support
Macmillan Cancer Support (quoting them) “improve the lives of people affected by cancer. One in three of us will get cancer, We are all affected by cancer. We can help. We are Macmillan.”
In 2011 Macmillan spent £106 million on services for people affected by cancer. They supported 1.7 million people with cancer and 640,000 carers. Of these they supported over 500,000 people through their Macmillan nurses and healthcare professionals who include nurses, doctors, consultants, radiographers, dietitians, clinical psychologists and others.
This is an organisation that has strong roots in providing comprehensive clinical health services to patients – a bit like the NHS really!
But in addition to their health and social care Macmillan also offer a range of financial help and support services. They know that 70% of people with cancer experience a drop in income or increased costs. In addition to grants they provide and commission a wide range of welfare rights services – many in partnership with their national strategic partner – Citizens Advice.
In 2011 together they helped almost 118,000 people and leveraged £200 million in benefits for them.
Why does Macmillan place more importance on commissioning services to tackle the social determinants of health than the NHS?
I think that there are two main reasons for this.
First – Macmillan does not have to account to Government for its spending. 98% of its income is generated through fundraising. This means that it is not tied to activities that are determined by government or by the (very limited and clinically dominated) evidence base. Instead Macmillan has to be able to convince its independent funders that the people who rely on its services value them.
Second – Macmillan is directly in touch with the people who receive its services and it listens to what people with cancer say they need. Through this Macmillan knows that access to financial support is key to the wellbeing of people with cancer, their families and their carers. This is sufficient evidence to give them the confidence to invest in welfare support services AND to give approximately 9% of their income directly in grants to people with cancer and their carers.
Implications for Commissioners.
- How do you recognise the impact of long term conditions on peoples wellbeing – and in particular the social determinants of health like income?
- Do the organisations you commission take responsibility for the whole person or are they only interested in them as site of a clinical illness?
- How much flexibility do you give to provider organisations? Do you prescribe the interventions and services that provider organisations should deliver – or do you block fund them and hold them to account for their expertise and their relationship with the people who depend on their services?
What do you think?
One of the risks of making something statutory is that times change and what  seemed like a good idea becomes at best a distraction and at worst an impediment. I wonder if we are beginning to see this with Joint Strategic Needs Assessments.
seemed like a good idea becomes at best a distraction and at worst an impediment. I wonder if we are beginning to see this with Joint Strategic Needs Assessments.
I think that we are beginning to see a growing dissonance between on the one hand Department of Health requirements to produce a Joint Strategic Needs Assessment, a Joint Health and Wellbeing Strategy, the various outcome frameworks and on the other hand approaches developed by local leaders to tackle tricky issues like health inequalities.
Ironically the big driver here is governments promotion of localism and citizenship.
The problem with many JSNA is that they start from the premise that is possible to build plans upwards from a rational assessment of need. I think that this approach is mistaken – it ties up scarce and precious analytical resources in a sisyphean task – and produces a product that is often still too siloed in health, is too complex for most to connect with and is by its nature too often reduced to a set of rather bland statements that have little impact on commissioning.
The JSNA problem
- Starts from the assumption that we need a complete picture of what a place looks like first in order to make rational decisions about investment. Leading to rather bland statements about action.
- Engagement is weak – usually starting with technical data experts then inviting others to comment on their work
- Siloed – struggling to adequately connect health and wellbeing to the wider determinants
Unsuprisingly agencies and organisations on the front line in particular find it hard to engage with this technical process of dubious impact.
Tackling the Social Determinants – the Commission Model
Increasingly local authorities are developing new models to drive commissioning that incorporate evidence, intelligence and citizens voice in ways that bring genuine challenge. one of the most promising are “Commissions”.
The approach here is different. The starting point is usually one where local politicians have made a decision to investigate a pressing and wicked issue and have asked for evidence and ideas about how to address this. Commissions recognise that the answers and evidence are just as likely to come from the front line and citizens as from ‘experts’. Indeed successful actions depend on all stakeholders being involved in problem solving.
Characteristics of a good commission approach include:
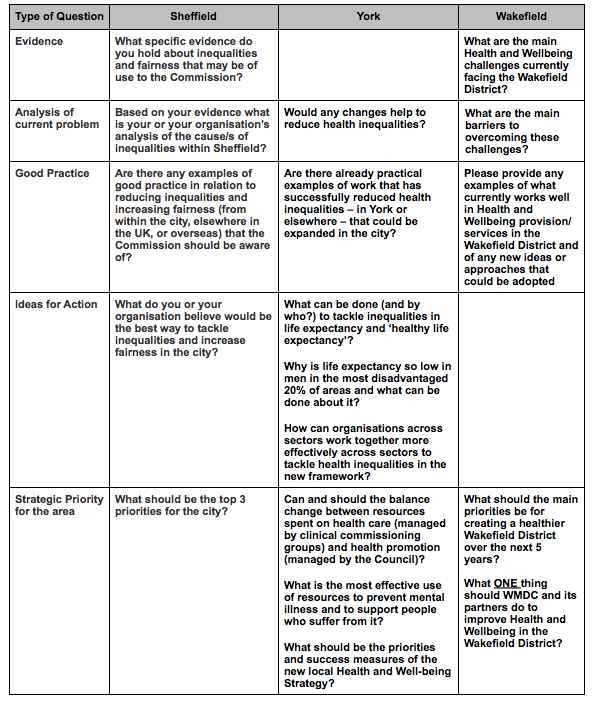
- Engagement of leaders and communities from the beginning – its interesing that commissions are able to engage a much wider group of stakeholders than health and wellbeing boards – have a look at the core membership of the York Commission and also at the broader group of stakeholders who are involved.
- A recognition from the outset of a key strategic challenge – a wicked issue – that needs addressing – by going public on the issue local leaders expose themselves to debate about whether they have chosen the right area and area and are able to engage local press and the public about why they have prioritised this.
- Clarity about the key questions that need to be addressed and an inclusive approach to capturing quantitative and qualitative data – see the table below for examples.
- Time limited and quick
- They locate Health Inequalities in a wider determinants agenda. None of the commissions set out to reduce health inequalities as the core objective – they are built around a broader notion of fairness and equity. This feels the right way round – and the connection with other social determinants feels more natural and powerful.
There are already a number of examples of these and it is not suprising that one of the key players is the Equality Trust – the organisation established following publication of the Spirit Level.
Here are 4 Commissions that I am aware of:
Islington – Fairness Commission
Wakefield – Poverty and Prosperity Commission
York – Fairness Commission
Sheffield – Fairness Commission
Strategic Questions
Here are some examples of the sort of questions that the commissions are asking – the grouping is mine – you may disagree
Conclusion
The commission approach feels the right way round with:
- Leaders taking responsibility for the problem and setting out a vision.
- Valuing different perspectives and views – and using a variety of evidence
- Multilayered opportunities for engagement and debate
- Generating an informed view across different stakeholders of actions that need to happen
What do you think?
Healthwatch – Getting Practical
Practical Action on Healthwatch
The recent helpful document – “Building successful Healthwatch organisations” produced by the LGA, Regional Voices and the NHS Institute starts at long last to put a bit of meat on the bones of what has, up until now been a process strong on rhetoric and weak on practicalities.
The “10 top tips” in the document focus mainly on how local authorities and their partners should manage the development process. The 15 case studies that follow start to give a feeling for the ambition of commissioners and the shape of the services that are being developed.
The case studies (10% of local authorities in England) are a mixed bag. They fall into the usual three categories – some really good ones, those that are still thinking things through – with a bit too much of a focus on organisational forms – and 2 or 3 that are embarassingly bad. I am not going to finger the ones that I think are bad – but frankly any place that claims to already have the model sorted and to have an existing organisation that provides an excellent service immediately sets off warning bells for me.
The ones that I thought were the most useful – in order of importance are:
- Lambeth – a strong focus on outcomes and a real clarity about a citizen led model
- Kent – very strong on the need for a powerful analytical function – providing the evidence to support strategic challenge
- Hertfordshire – Importance of effective capability for investigations and the need for real expertise in community infrastructure.
- Staffordshire – Interesting research following quite large scale consultation – although model not clear
Anyone close to Healthwatch will understand just how difficult the task is – as we struggle to come up with a powerful engaged whole system model of citizen led quality assurance with real clout but limited resources.
The table below sets out some of my thinking – looking at some of the imperatives and the service and capability that might be required. This is very much work in progress!
Of course what it does not show is how the service should be structured and the relative balance of investment across the different functions. Please comment on it!
Whole System
A final thought -this is not just about commissioning Healthwatch and then saying the job is done – I think this is one of the reasons that LINks struggled so much. The local commissioning system has to build the role of Healthwatch into how it works. Health and Wellbeing Board members will need to champion local Healthwatch outside meetings – as well as changing their organisations behaviours – for example – building in a requirement to engage with Healthwatch into the contracts of all local providers – including GPs.
Department of Health – Public Health Workforce Strategy – Puts the general public in the driving seat!
“It is essential that the general public is in the driving seat for all aspects of their own health and wellbeing……..This approach emphasises what people can do rather than what they cannot”
 The problem of course is that the above statement appears at the bottom of page 27 of the consultation document “Healthy Lives, Healthy People: Towards a workforce strategy for the public health system (TaWSPH). In order to get to this “essential” part of the strategy we have to wade through:
The problem of course is that the above statement appears at the bottom of page 27 of the consultation document “Healthy Lives, Healthy People: Towards a workforce strategy for the public health system (TaWSPH). In order to get to this “essential” part of the strategy we have to wade through:
- irrelevant questions – how often should we renew a workforce strategy – should it be every 3 years or every 5?” (p10)
- unchallenged assumptions – “at a time of change it is essential to focus on sustaining the specialist workforce” (p12) – why? Or – “Public health specialist and practitioners should be subject to quality assured enumeration” (p12) – why?
The reason for the above approach is clear – while the public health profession continues to aspire to a role of national significance – it still assumes that the most important audience are the current inhabitants of the Public Health Village – primarily members of the Faculty.
What is most concerning though is that the consultation document seems to have been written in isolation – failing to recognise the demographic, socioeconomic, practice and policy challenges that contemporary public health faces at the moment.
Reading this document it is not possible to get a feeling for how big the challenge facing the public health workforce is or indeed the scale of ambition to transform it. The executive summary states that “the current changes to the public health system will have a significant impact on the public health workforce and will lead to a new system of delivery that will need new skills and new ways of working” (page 6). This is not really explained – but the impression that is created is that the challenges are organisational ones – transfer to local government, creation of Public Health England etc. There is an absence of context and analysis about what is currently working or not.
The economic and policy context
Helpfully on page 9 TaWSPH draws attention to the Local Government Workforce Strategy which is called “Delivering through People”. This provides a strategic analysis of the context and challenges that will face public health as it moves over to local government. Here are three key quotes from the foreword.
- ‘The most critical issue currently is addressing the workforce dimension of major service and organisational transformation. With partners, councils are reconfiguring local public services to ensure that they achieve priority local outcomes with significantly less resources.”
- “If we ever had the ‘burning platform’ required to make major cutural changes, we have it now.
- “We need to tackle the difficult issues that get in the way of setting up new organisational structures, such as professional rigidity ..”
In the section on context (p6) the document sets out some of the key challenges:
- Councils face an unprecedented period of declining resources and growing demand
- This is driving customer focused service transformation and innovation
- Well established professional disciplines and practices will need to be reviewed and updated
So the local government environment is one where services are being cut, salaries have to be justified and existing roles questioned – any workforce strategy must acknowledge this context – TaWSPH fails on this count.
The practice challenge
In addition to the economic and policy context described so clearly in ‘Delivering through people” Public health also needs to look very critically at its current delivery model. There are strong arguments that it is currently not fit for purpose – particularly with regard to its impact on key issues such as health inequality, obesity, mental health and the social determinants.
In Nigel Crisps (ex Chief Executive of the NHS) book – “Turning the World Upside Down – the search for global health in the 21st Century” which Simon Duffy at the Centre for Welfare Reform brought to my attention Crisp elegantly sums up the challenge:
“The core features of western scientific medicine are:
- greater professional competence
- scientific discovery
- commercial innovation
- massive spending
Crisp states that all these core features )which have some similarity with the public health vision described on page 9 of TaWSPH) need to be turned upside down as part of a paradigm shift:
- greater professional competence is achieved through patients and communities empowering and working with professionals
- Scientific discovery is made relevant by our understanding of society and how to apply it
- Commercial innovation is effective only as part of wider goals
- measures of input spending are replaced by measures of social and economic value achieved”
Three challenges that the workforce strategy needs to address.
Impact – It has to keep a focus on reducing health inequalities at a time of huge challenge. The starting point must be a robust assessment of what has worked well and what has not. This document reads too much as though the purpose is the defence of the public health specialist.
Citizens in control of their health – there needs to be a fundamental rebalancing – focussing on public healths contribution to co-producing solutions with communities. This is not an add-on – which is how it feels in this document. We need to re-balance our approach to put community leadership at the heart of this work. There are plenty of examples already – such as Well London, Altogether Better and the Health Empowerment Leverage Project (HELP).
Public Health Leadership – the workforce strategy needs to recognise that leadership for public health now rests with local government. So the leaders of the public health system are Cabinet Leads for Health and Wellbeing and Local Authority Chief Executives. Their role needs to be formally acknowledged in the broad groupings of public health that are used (p14 of TaWSPH)
What do you think?
A month ago I shared a platform with Ruth Hussey at an East Midlands Public Health event. One of the points that Ruth made was about how good some of the public health websites were in the United States. This is important – after all public health has to:
- influence leaders across the whole system from clinical to social determinants
- provide information for the public and professionals
- help people access key public health services
- enable citizens to become more active with regard to their own health as individuals and concerned citizens.
The way an area sets out its approach to public health through a web site is a good indicator of:
- how coherent the approach is
- who is actually involved and engaged
- the degree of commitment to involving non-professionals
Public Health in America
I searched on google using the term “public health + name of city”. Here are three links to American public health websites:
Here is what I found – in general they:
Are owned by politicians
Strong political representation – its clear who the lead politician is and their interest in this agenda.
Show Public Health in the round:
- Information about how to access services
- Information about 3 domains of public health
- Information about strategies and need
- Information for citizens about how to improve their health
Are up to date
- Accessible news feed
Have ways for citizens to get involved
- You tube
- email contact
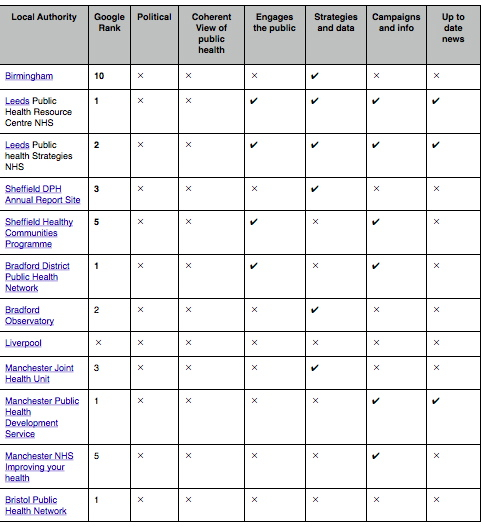
So on the basis of the above I created a set of criteria and used these to rate the public health websites of the six biggest (by population) local authority areas in England.
As with the USA I have only used the search term “public health + local authority name”
The first challenge is that the search term I used did not always identify a website. In some cases (Birmingham and Liverpool for example) it was hard to find any coherent website.
I realise that there may be some fantastic websites that I have missed because I have only searched under this one term. My counter argument would be that any well used website, should be using the tag “public health” and would be picked up by my search.
I have tried to be fair and where more than one website has come up in the top 5 on google I have included that as well.
The Criteria:
- Google Rank – what position did the website appear on the google page – if it was first it is ranked 1 etc.
- Political – is their clear ownership by local politicians – statement from the cabinet lead for health or their name.
- Coherent view of public health – the scope of the public health agenda is represented across all three domains – health protection, health improvement and social determinants of health.
- Engages the public – there is an easy way for citizens to sign up for more information and their involvement is encouraged.
- Strategies and Data – key strategies and data is available – DPH Annual Report, JSNA, etc.
- Campaigns and information – information about public health campaigns available.
- Up to date – there is a news feed that has news on it that is no more than 1 month old.
Two types of organisation appeared more consistently than local public health departments. These were Academic Institutions and Public Health Observatories. This is probably because they are committeed to being outward facing – to promote their work and attract students in the case of universities and to share their data and intelligence in the case of PHOs. Local Public Health Departments could learn from this approach.
Strategies
The one area of comparative strength is that most of the websites surveyed did provide access to some local public health strategies and the JSNA.
Incoherent
Most areas surveyed do not have a coherent public health portal with public health services scattered across different websites – making it hard to see the connections between different services and approaches. There is a lack of consistency of leadership across public health agendas with a siloed approach – NHS, Community and to an even lesser degree local government.
Citizen Engagement not prioritised
In general there is little interest in presenting clear ways for citizens to engage in the public health agenda. Where attempts have been made to do this they often feel poorly resourced and evidence a lack of long term commitment and direction. (see this Sheffield site – which has 203 health ‘pledges’ – Sheffield is a city of over 600,000 people!). In general the assumption of most websites appears to be that their primary audience is fellow professionals.
Dead websites
Too many websites are ‘dead’ with few opportunities for interaction, no live news feeds and evidence that they have not been maintained for some time. For example Liverpool First for Health and Wellbeing does not appear to have been updated for at least a year.
Lack of connection with local politicians
No website demonstrated that public health services had strong political connection with the relevant cabinet lead for health. This probably is a reflection of the fact that the leadership role for public health is sometimes assumed to stop with the the Director of Public Health – the Sheffield DPH website in the table above is a good example of this. We would not expect to see a Director of Adult Services or Director of Housing having their own website – local politicians need to step up and own this agenda.
Conclusion
To be frank the more I have looked at these websites the more concerned I was at the insular approach that public health has taken so far. Particularly with regard to engaging with citizens and working with local politicians. The move to local government presents a real opportunity to make progress here. However, it will be important to acknowledge that existing approaches for connecting and engaging with the wider workforce and local citizens are not fit for purpose.
Finally – as usual let me know what you think:
- are there some other criteria I should have included?
- do you know some great public health websites that you think we should know about?
- do you know of some terrible ones we should use as examples of how not to do it?