HealthWatch – Rhetoric and Reality
 I have 3 concerns about the Department of Health publication Local HealthWatch – the policy explained (LHWtPE) which came out earlier this month. These are: the critique of LINks; the absence of public health and the emerging remit for HealthWatch.
I have 3 concerns about the Department of Health publication Local HealthWatch – the policy explained (LHWtPE) which came out earlier this month. These are: the critique of LINks; the absence of public health and the emerging remit for HealthWatch.
Concern 1 – The Critique of LINks
The document starts (1.3) with a hard nosed critique of LINks.
Stating among other things that:
- LINks found it “impossible to be truly representative of their local population.”
- LINks showed “unecessary variation in ways of working and effectiveness.”
- the public and health and care professionals were unaware of the work of LINks and they lacked a consistent identity
- there is no no national organisation to provide consistent identity
Some of these statements may be correct – but no source is given. It is not acceptable for this sort of unsubstantiated critique to appear in a Government policy document.
Further some of these statements feel like rather crude rhetorical flourishes – precisely what is meant by “truly representative of their population?” This phrase is used a number of times in the document. Are there examples of services that are consistently truly representative against which we can benchmark the performance of LINks? The NHS Commissioning Board perhaps? Maybe the boards of Hospital Trusts? Perhaps the Executive Team of the Department of Health?
I am not disparaging the ambition here – just pleading for a bit of sophistication and clarity.
Another example – “unecessary variation in ways of working and effectiveness”. Again what level of variation is unacceptable? How does the degree of variation of LINKs compare to variation in say NHS services for children where there is a more than 3 fold variation in A&E attendance for the 0-4s? or quality of homecare? The 2011 NHS Atlas of Variation notes that “it is common to see twofold or greater difference in PCT expenditure for each programme budget area” (page 19). How does the variation among LINks compare to this?
What is most disappointing is that there is no recognition in this or any other documents of the challenges that any agency that is charged with bringing challenge and criticism to local systems has to face. Anyone who has worked in the local statutory sector will have heard senior managers often talk defensively, disparagingly and critically about organisations like CSCI, CQC and the Audit Commission. This is the environment that LINks have operated in and that HealthWatch will enter. Policy documents such as LHWtPE need to show some awareness of this. LINk/HealthWatch managers will require very sophisticated influencing skills, a strong grip on principles, the pragmatic negotiating skills of ACAS and the skin of a Rhino.
You can see the point – the analysis as presented is a straw man – knocking down LINks in order to justify the establishment of HealthWatch and its relationship with CQC.
Concern two – the Department of Health forgets Public Health
In March 2011 the HealthWatch Transition Plan (HWTP 2.13) says that “Local HealthWatch needs to develop a good understanding of what good looks like in the public health arena” it goes on to state that “the Department of Health will continue to work with public health colleagues and with councils and LINKs (HealthWatch) to help determine what information and evidence HealthWatch will need and how they can best get it and use it.
It states (HWTP 2.16) that “one key element for realising the (Governments) visions for the NHS, public health and adult social care is the establishment of …. HealthWatch.
There are further references to public health with regard to bringing forward the views of the public (HWTP 2.31) and in relation to the analytical capacity that HealthWatch will need to have.
The HWTP (2.19) also makes clear reference to HealthWatch giving “local communities a bigger say in how health and social care services are planned, commissioned, delivered and monitored to meet the health and wellbeing needs of local people and groups and address health inequalities.
One year later all references to Public Health and health inequalities have gone. In LHWtPE The only reference that comes close is a reference to health improvement in the context of local authorities roles.
So, the remit of local HealthWatch has become narrower – it is now almost exclusively focussed on a service access and quality role – focussing on the provision of NHS and Social Care services.
This stands out even more when we look at the roles, responsibilities and functions of local HealthWatch (LHWtPE 4.1). Which are clearly focussed on health and social care services.
Any notion that local HealthWatch would have some room for manouvre with regard to bringing the citizen voice to the debate about the balance between downstream clinical and care provision and upstream work to address the social determinants of health seem to have gone.
So, the contribution that Healthwatch could have made to bring citizens in to help commissioners tackle one of their most difficult challenges – rebalancing expenditure to focus on prevention has been substantially weakened.
Final Question – so what is the purpose of HealthWatch?
When I look at what remains of the HealthWatch remit it feels as though it is increasingly boxed into a corner – it feels rather anodyne and has a slight taint of PALs.
This narrow role of local HealthWatch is summarised by David Behan in his “Dear Colleague” letter of the 2nd of March as:
“Giving citizens greater influence over local health and social care services and to support citizens access information about the increased choices available to them under the reforms.”
The future success of local HealthWatch rests with the way in which local authorities will choose to commission it.
A first step is to consider what the two functions that David Behan sets out actually mean in commissioning terms.
Support citizens access information about the increased choices available to them.
This could be interpreted as signposting and advising people about services. I have seen no evidence produced by the Department of Health of exactly what the deficit is that needs addressing. I am unclear about the added value that a small service can provide on top of the responsibility that local government and the NHS already have to ensure that their services are accessible and people get the advice they need about which ones to use.
Local Commissioners will need to consider:
- Precisely what is the added value that they need local HealthWatch to bring here?
- What is the relationship between this service and other local signposting and advice services?
Giving citizens greater influence over health and social care services.
The remit now feels much narrower – focussing on social care and health services not citizen engagement with wellbeing. In many cases it is not how we experience individual services – but how they interact or don’t that is the issue. For example – mental health, housing and utilities. There is a strong argument that sophisticated generic advice and advocacy services like Citizens Advice are best placed to respond here.
Local Commissioners will need to consider:
- Do they want to commission local HealthWatch to have a broader role that allows citizens to engage on wellbeing and social determinants issues rather than the narrow one described by DH?
- Do they want HealthWatch to challenge and develop how commissioners and providers engage citizens or do they want local HealthWatch to provide the engagement?
- What is the relationship between any processes that local HealthWatch might establish and other mechanisms (neighbourhood committees for example) that already exist?
Old JSNA – New JSNA
I recently ran a workshop for Sarah Salway’s team at Sheffield Hallam University on embedding ethnicity evidence in Joint Strategic Needs Assessments. This is part of a piece of work they are responsible for on Evidence and Ethnicity in Commissioning.
While preparing for the workshop it struck me that with any new initiative we tend to focus on the present and the future rather than considering how this relates to what we did in the past. At times of transition I think it is important to understand our past context so that we can change our behaviours, cultures and expectations to fit the new environment.
I have put together the ‘handy table’ below that tries to capture this – let me know if I should add more – or if you disagree with it!
You can download a copy of the table below here – Old JSNA – New JSNA MG
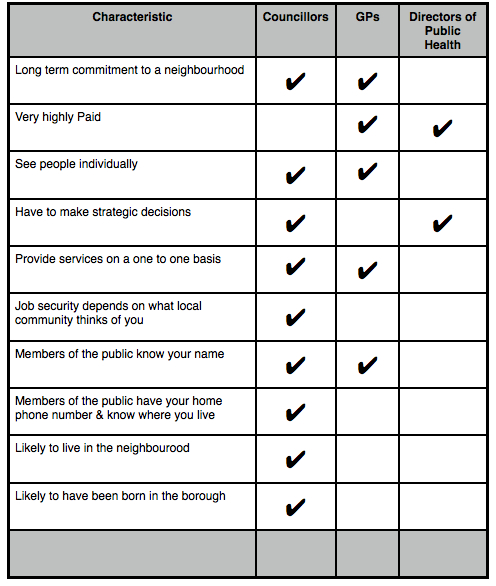
Friends or Enemies? What have Councillors, GPs and Directors of Public Health got in common?
As public health moves over to local government and Health and WellBeing boards are established some of the key players need to understand each better. Here is a quick list that highlights some similarities and differences. With thanks to some (anonymous) colleagues of a well known national organisation.
By the way – I have not put GPs down as being responsible for making strategic decisions – this is because I am still not convinced that ALL GPs will be personally making strategic decisions that affect whole populations – this is something that Councillors and DsPH are of course already responsible for.
What are your suggestions for similarities and differences – let me know and I’ll add them to the table.
You can download a copy of the table here – Table – Cllr; GP; DPH
Healthwatch set up to fail?
 Two important documents have been published by the Department of Health which focus on the role of Healthwatch England.
Two important documents have been published by the Department of Health which focus on the role of Healthwatch England.
The first is a ‘Healthwatch Narrative’ which explains the thinking behind the establishment of Healthwatch England and provides the context for the second which is a consultation on the composition of the Healthwatch England Committee.
The Healthwatch narrative.
This starts with an assertive justification of Healthwatch England.
Note – 3 overhauls in the last 9 years. This is a service whose role relies on a strong relationship with citizens!
It goes on to say that LINKs have encountered a number of issues (I paraphrase):
- no national body to provide leadership
- they have tended to be unrepresentative
- there has been too much variation and insufficient peer support
- they lack a profile and have no consistent identity which has hindered success and reach
We don’t take citizen led improvement seriously enough
If the above analysis is correct then why have local commissioners and PCTs and their national bodies – LGA, Strategic Health Authorities and NHS Confederation consistently failed to address this deficit?
This is probably because local commissioners have seen the contribution of LINKs and its predecessor CPPIH as marginal to improving the quality of services and therefore not worth bothering about.
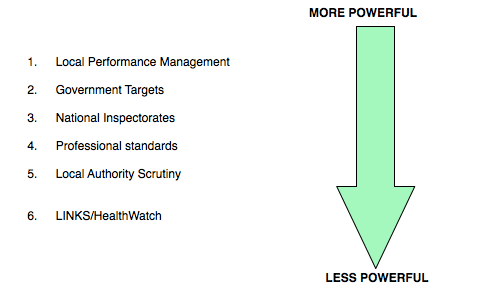
I think that the current paradigm for quality and improvement drivers probably looks a bit like this:
LOCAL DRIVERS FOR QUALITY AND IMPROVEMENT
More problems
The establishment of a national Healthwatch Committee is clearly an attempt to address this weakness. However there are further challenges. Here are three:
First – Remit
The summary list of Healthwatch pathfinders came out in October 2011. This lists the topics chosen by the 75 Healthwatch pilots – the diversity of interests and variation in focus is tremendous. This is despite the fact that leadership for most of the pilots rests with local authorities rather than with LINKs – so we might reasonably expect strong strategic direction.
While it could be argued that this diversity reflects local priorities and agendas it is as likely to be an indicator of:
- a lack of engagement at a strategic level in local government – leading to a lack of strategic focus for the HealthWatch pilot
- a mismatch between the scale of the Healthwatch role and the resources currently available – leading to a lack of clarity about mission
- a lack of connection with other approaches to engage citizens at a local level – leading to a siloed approach to an issue that is should be central to all of us – health and wellbeing.
- A reluctance to move from the improvement paradigm I have described above to one that places a greater emphasis on citizen led accountability.
Second – Everything and Nothing
The Healthwatch transition plan identifies Local Heathwatch as the ‘local consumer voice for health and social care’ and sets out its remit as:
- Influencing – help shape the planning of health and social care services
- Signposting – help people access and make choices about care
- Advisory – Advocacy for individuals making complaints about healthcare.
However elsewhere in the literature we also see reference to:
- (Inspection?) – ‘it will also have a remit for adult soial care services including rights to entry to premises where care services are provided’ (page 13 transition plan)
- Public Health ‘local Healthwatch has a role in promoting public health, health improvements and in tackling health inequalities (page 7 DH Narrative)
- Accountability – ‘through Healthwatch, people will be able to hold the new system to account’ (Healthwatch narrative – page 13)
There is a real risk of role confusion, being spread too thin, losing strategic focus etc. Healthwatch has to:
- Signpost people to health and social care services
- Come up with sensible challenge on the quality of health and social care services
- Be an advocate for public health, health improvement and public health.
The danger is that the wicked issues where we have made least progress – public health, health inequalities – will continue to be poorly served and the more traditional areas – right to entry etc will get more attention.
This challenge is not specific to Healthwatch – other advocacy organisations such as Citizens Advice know all about this struggle to get the balance right between responding to individual need and making an impact on policy at a local level – and Citizens Advice has a narrower remit than Healthwatch!
Third – Incorporation
Appropriately DH has chosen to keep the local authority scrutiny function separate from the remit of the Health and Wellbeing Board. This will lessen conflict of interest and the risk of incorporation.
Yet Healthwatch has a statutory place on the Health and Wellbeing Board. At one level this seems reasonable – an ambition by government for an inclusive and co-produced approach – it feels like a validating quick win for new local Healthwatch. However, membership of the Board brings formal and informal accountability to this group. It has real potential to limit the room for manouvre of local Healthwatch – making it harder to articulate in public a view that is independent of the Health and Wellbeing Board.
This tension is described in more detail in a good piece by Professor Jonathan Davies on the NCIA Website (For Insurgency: The Case against Partnership : Independent Action)
So, legislators may feel that they have assurred a positive, welcoming and inclusive seat for Healthwatch on the Health and Wellbeing Board but their positive intentions could actually be seen instead as rather naive policy making – coming before sound design; constraining local authorities and risking weakening the impact of Healthwatch rather than strengthening it.
It would have been better for Healthwatch to have a clear remit to support and strengthen local authority overview and scrutiny arrangements which are generally poorly resourced.
What Local Authorities can do
The role of Local Authorities is key here – they will commission the new service. They face a very tough environment and urgently need resources that will help them engage with citizens to defend good local services, challenge services that are not performing and in particular promote a community led – as opposed to clinician led health and wellbeing delivery model.
A good local authority will commission a Healthwatch service that is able to clearly articulate the view of citizens even if these may sometimes feel uncomfortable for local government.
Commissioning arrangements that bring Healthwatch closer to working with scrutiny committees would be strong.
Using some Healthwatch resources to build citizen led intelligence functions and capacity building would also help – as I set out in an an earlier blog on this subject.
There are strong lessons from a diverse range of sources such as:
Constructive Challenge – Citizens Advice, the Tenants Movement, DH National Support Teams about how to bring constructive challenge.
Building Capability of Citizens – LMU Institute for Health and Wellbeing, Altogether Better England, Workers Education Association
What DH and Healthwatch England can do
The creation of a dynamic, independent and challenging organisation is not going to be determined by deciding who sits in which deckchair.
There are a wide range of examples within the voluntary and community sector of how relationships between national and local bodies can bring innovation and energy as well as trouble and destruction.
The Department of Health and CQC should urgently hold some tight discussion groups with organisations who have long experience of managing the relationship between local organisations and a seperate national one. Organisations which operate a federated structure with a strong citizens base have a lot to offer such as:
What do you think?
A PDF of this blog is available here: healthwatch discussion paper
Latest on Inclusion Health
Well since writing my blog on ‘Whatever Happened to Inclusion Health’ I have  come across some more information. Hopefully some of this material will be available officially soon – but in the interim…..
come across some more information. Hopefully some of this material will be available officially soon – but in the interim…..
The Lead Minister is Ann Milton and the board members are as follows:
Professor Steve Field – Chair of National Inclusion Health Board
Sir David Nicholson – Chief Executive NHS Commissioning Board Authority
Professor Sir Michael Marmot – Director, International Institute for Society and Health and MRC Research Professor in Epidemiology at University College London
Cllr David Rogers – Chairman of the Local Government Group’s community wellbeing board and Vice chairman of East Sussex’s health overview and scrutiny committee.
Charles Fraser – CEO St Mungos
Professor Lindsey Davies – President of the Faculty of Public Health
Sandie Keene – Association of Directors of Adult Social Services (ADASS) National Lead on Public Health and Director of Adult Social Services in Leeds – and from 2013 President of the ADASS
So – we have a board made up of a tremendously powerful group of players – this should mean that we can expect significant leadership on this agenda from at least four key organisations/federations which have a national reach:
- National Health Service Commissioning Board
- Association of Directors of Adult Social Services
- Local Government Group
- Faculty of Public Health
I think it is really important that the existence and aims of this board are brought to the attention of elected members, paid officers, professionals and community leaders who are concerned about meeting the needs of excluded groups.
The priority groups that Inclusion Health is focussing on are:
- Sex Workers
- Vulnerable Migrants
- Gypsies and Travellers
- Homeless
Priorities
The board has established 4 main working groups and have appointed the following leads:
- Leadership and workforce: This working group will focus on getting Inclusion Health embedded within postgraduate training and developing leaders in the field that lead by example on Inclusion Health. This will be led by Rosemary Cook, Director of the Queens Nursing Institute.
- Data and research: This working group will focus on strengthening the collection of robust data and comprehensive research on the groups identified in the Inclusion Health programme. This will be chaired by Dr Bobbie Jacobson of the London Health Observatory.
- Provision, prevention and promotion: This working group will focus on gathering models of good practice. This will be chaired by Dr Nigel Hewett member of the University College London Hospital Homeless Team.
- Assurance and accountability: This working group will focus on how the system can be held to account on the Inclusion Health programme. This will be chaired by Professor Helen Lester, Practitioner and Lecturer at University of Birmingham.
Action we can all take
There are many of us who have been trying to bring this agenda into the mainstream – after all its not just the four groups of people who are excluded – but by their nature the front line services who try to meet their needs – they also often lack profile and mainstream recognition.
So it is crucial that when opportunities arise we contact and talk with the members of the board identified above – with a view to supporting them and encouraging them to continue to keep focussed on this agenda.
Responding to the Joint Strategic Needs Assessment Guidance Consultation
This Department of Health Consultation ends on the 17th of February
In this note I am focussing on 3 areas that I think are the most important with  regard to Joint Strategic Needs Assessment (JSNA) and Joint Health and Wellbeing Strategy (JHWS). These are:
regard to Joint Strategic Needs Assessment (JSNA) and Joint Health and Wellbeing Strategy (JHWS). These are:
- Role of Local Authorities
- Purpose of the Health and Wellbeing Board (HWB)
- Resources
Purpose of the guidance
This is described as:
“intending to support health and wellbeing boards and their partners undertake and contribute to Joint Strategic Needs Assessments and Joint Health and Wellbeing Strategies within the modernised health and care system.”
Context
This is the Departments of Health view of context
“The Government has set out a new vision for the leadership and delivery of health and care services……central to this vision is that decisions about services should be made locally as possible, involving people who use them and communities to a maximum degree. Strong leadership is vital to this vision – local leaders will need to identify what the needs of the local community are and then establish how those needs will be met, either through the services they commission, or through joint working and collective action”
We know that at a local level the contextual imperatives are:
- An economic crisis
- Social Policy that is failing to protect the poor
- Cuts to local authority spending
- A funding crisis in Social Care and increasingly in the NHS
- A historical failure to reduce health inequality
- A government that promotes decentralisation but also runs things from the centre when it chooses to.
There is no point focussing on the technical aspects of the JSNA and the JHWS first – the effectiveness of these two processes will stand or fall on the leadership and vision of the Health and Wellbeing Board.
At a local level the buck stops with the health and wellbeing board and hence with the local authority which has lead responsibility for making this local system work.
If the local authority does not get the local structures right, set the right tone and vision then all the notions of inclusiveness, good practice for JSNA and JHWS are irrelevant – the JSNA and JHWS will remain the province of officers – and probably fairly junior ones.
So its worth starting by looking at the Annexes at the back of the document which set out the duties of respective bodies and in particular what local authorities can do.
What local authorities can do
Annex B states that:
- It is for the local authority to determine the precise number of elected members on the board, and it is free to insist upon having a majority of elected members
- When establishing the HWB the local authority can determine the initial membership
- Once the HWB has been established the local authority may change the composition of the HWB subject to consultation with existing members.
There are strong reasons for local authorities to move straight to creating boards where the majority are elected members – or at the very least where they are the largest group.
Arguments for elected members being in the majority on Health and Wellbeing Boards.
- local authorities will be held to account for the performance of the HWB therefore they need have a strong grip on the board
- it is a clear indication that the local authority is taking the HWB seriously – in effect treating it as a council committee
- it changes the culture of the board to one that is more in tune with a committee led by politicians than officers
- it provides the opportunity to bring a much greater emphasis on community and the social determinants of health from the beginning.
Arguments against:
- the amount of elected member resource required
- handling issue – it could be percieved by other members as a take over by local authorities rather than as a manifestation of leadership and ownerships.
Inclusive Health and Wellbeing Boards
Given that it is for local authorities to determine the initial membership – beyond the minimum requirements – they will set the tone for the degree of ambition with regard to improving health and wellbeing.
A narrow membership at the start will mean a narrow view on who is responsible for improving health and wellbeing and will keep the discussion focussed on how to manage the existing health and social care spend and providers rather than shifting towards a stronger upstream focus on the social determinants of health.
One of the challenges that local authorities will face is how to build stronger alliances with community based interests who are focussed on addressing the social determinants of health.
Bringing these organisations and sectors onto the health and wellbeing board will be necessary if resources and plans are to refocus on community and prevention rather than on acute and reactive.
It is probable that some of the more enlightened members of Clinical Commissioning Groups would see this approach as empowering. If a new localist commissioning agenda is to be developed that focusses more on the social determinants of health this will require the conscious creation of a new culture and way of thinking on the HWB.
It will be important to have allies around the table who can work together to validate this agenda.
So, we should expect to see a significant membership drawn from sectors such as Housing, Welfare Rights, Careers Services (if the government has not cut them all), Education etc. Of course some of these could be elected members themselves.
The need to take this approach is reinforced in paragraph two of section 5.3 wich states that:
“HWB has the power to request that the LA, CCG, HW, NHSCB or other HWB members supply information for the purpose of undertaking JSNA and JHWS – and these partners must supply the information as requested”
In other words local authorities should put organisations on the HWB who bring broader sectoral interests with them and whose information they require.
If they are not on the Health and Wellbeing board their data will be harder to access and the JSNA and JHWs will be narrower.
Resources to produce the JSNA
CCG and Local Authorities will each have equal and explicit obligations to preapare a JSNA (4.1.1)
What this means
CCGs and Local Authorities have a shared responsibility to equally fund and resource the analytical capability to deliver a JSNA and to discharge it through the HWB.
Action required
Local Authorities should urgently be capturing the analytical, strategic and involvement cost of producing the JSNA and ensure that the CCG is making an equal contribution in time and finance to its production.
The rest of the guidance
The rest of the guidance is focussed on a range of technical matters – who reports to whom, principles of what a good JSNA is etc. Much of this is either technical or affirms what is already understood. It all stands or falls on the 3 issues described above.
Whatever happened to Inclusion Health?
 In these nasty times as the government tries to divide us into the deserving and undeserving – organisations who support some of the most excluded need all the help they can get. There is an existing Department of Health/Cabinet Office programme “Inclusion Health” that should be empowering champions in this area – but it has little profile at the moment. Why is the Department of Health not promoting it more assertively? I was reminded of Inclusion Health when reading one of the NHS Future Forum Publications and came across a reference to it tucked away on page 27 of the “NHS role in the public’s health”. It’s not surprising it’s there; as well as being the NHS Future Forum Czar Steve Field is also responsible for Inclusion Health. Inclusion Health was commissioned by the last Labour Government and due to the championing of Steve and some excellent civil servants it survived the change of Government and has been endorsed by Ann Milton (Hansard column 755 18th Oct 2011) – the current Parliamentary Under Secretary of State for Public Health. It focusses on looking at ways to improve the health of some of the most easily ignored groups in society. People whose health outcomes are far worse than the England average – they include:
In these nasty times as the government tries to divide us into the deserving and undeserving – organisations who support some of the most excluded need all the help they can get. There is an existing Department of Health/Cabinet Office programme “Inclusion Health” that should be empowering champions in this area – but it has little profile at the moment. Why is the Department of Health not promoting it more assertively? I was reminded of Inclusion Health when reading one of the NHS Future Forum Publications and came across a reference to it tucked away on page 27 of the “NHS role in the public’s health”. It’s not surprising it’s there; as well as being the NHS Future Forum Czar Steve Field is also responsible for Inclusion Health. Inclusion Health was commissioned by the last Labour Government and due to the championing of Steve and some excellent civil servants it survived the change of Government and has been endorsed by Ann Milton (Hansard column 755 18th Oct 2011) – the current Parliamentary Under Secretary of State for Public Health. It focusses on looking at ways to improve the health of some of the most easily ignored groups in society. People whose health outcomes are far worse than the England average – they include:
- Gypsy and Travellers – only 30% of Irish Travellers live beyond 60
- Homeless People – consume 8 times more hospital inpatient services than people of a similar age and are 40 times more likely not to be registered with a GP
- Street Sex Workers – over 80% report using heroin or crack cocaine
- Adults with a learning disability – 58 times more likely to die prematurely than the general population
Some really good work was done on the evidence and on working out what action could be taken. Much of this work is summarised in “Inclusion Health – How we meet the primary health care needs of the socially excluded” This is where the data above comes from. You will note that the only version I can find on the web is the ‘Labour Government’ one. Some of the actions described emerged from collaborations between organisations such as hospital trusts and the voluntary sector. There is a case study that gives a great insight into this on page 12 of ‘Integration’ another NHS Future Forum Publication. A slightly abridged version of the case study is here – with highlighting by me: “Jim and the London Homeless Pathway Jim was brought into A&E at University College Hospital (UCH) in London with alcohol withdrawal seizures and malnutrition, having been found by paramedics collapsed in the ground floor common room of his hostel where he had been unable to climb the stairs to his room for two days. Upon admission, it was discovered that he also had alcoholic fatty degeneration of the liver, cerebral atrophy and symptoms of cerebellar ataxia and peripheral neuropathy (alcohol related brain and nerve damage); he also had many old scars of self‐harm. The usual practice would be to get Jim back to his “baseline” and discharge him as rapidly as possible back into the community. Since 1995 Jim had attended A&E at UCH 155 times; had been admitted to hospital 11 times and spent a total of 62 days as an in‐patient. Usually this had been related to self‐harm or alcohol‐related damage. Having been homeless for the last seven years with periods of rough sleeping, he had never been deemed to have social care needs and medical care had been reactive. All of his mental and physical health problems were dismissed as alcohol‐related. The London Homeless Pathway integrated service team befriended Jim, and arranged to replace his soiled clothes. Talking to him, it was clear that much of his agitation was due to ongoing alcohol withdrawal symptoms and an increase in the dose of his medication was negotiated. Instead of the usual rapid discharge, assessments were arranged with an occupational therapist and a physiotherapist. Jim was supported on a daily basis and involved in decisions about his care. His medical history and current findings were summarised in a report by the Pathway team GP and a referral to social services was made. The accumulated information clearly showed significant care needs and he was placed by the local authority in a residential unit, where he settled well and considerably reduced his alcohol consumption. Jim has not needed to attend A&E at UCH for over 12 months.” If you dig deeper into the story of the homeless pathway we see that it includes the use of peer volunteers (see section on Healing) who help medical and social services keep in touch with service users and helps prevent reactive crisis led responses. A few points.This work is exciting and important because:
- it recognises that complex challenges require integrated solutions involving a wide range of agencies and solutions
- it is positive and optimistic about individuals desire and ability to change
- it recognises the importance of listening to the client
- it understands the importance of being connected – and has worked out a way of involving volunteers to facilitate this.
- it has been initiated by those organisations who experience the problem – the providers of last resort – rather than the commissioners, primary care providers or public health. These are the organisations usually hospital A&E or front line voluntary organisations who people turn to at times of crisis when other services have ignored them.
But what about Inclusion Health? If you search the web for ‘Inclusion Health’ you will only find a few old references to this initiative. Apparently work is still going on– I understand this includes:
- A National Inclusion Health Board chaired by Steve Field I can find no public minutes or indication of when it last met. (I know he is a bit busy at the moment)
- Four working groups
- Working relationships have been established with representative organisations across 4 priority groups
- Updated Data Packs
- Support to two ministerial groups on homelessness (no record of activity since September 2011)and Gypsies and Travellers (I can’t find any public agenda or minutes for this group).
This is all tremendous stuff – but the most up to date public reference to Inclusion Health that I can find is from the 7th of July 2011 where Steve Field praises the launch of Grant Shapps’ “no second night out” which aims to reduce rough sleeping. Unfortunately on the 17th of October the National Housing Federation, Shelter and the Chartered Institute for Housing produced a pretty damning indictment of Government Housing Policy “The Housing Report” which gave a red traffic light progress on homelessness stating that: “…the increase in homeless acceptances and use of temporary accommodation is troubling.” The lesson is clear – To be credible Inclusion Health needs to be better at providing authoritative independent public challenge to government policy as well as support when it is merited. SO
- Inclusion Health is a really important initiative. It draws attention to the needs of people we ignore too easily and provides a template for action.
- Its is tremendous that it continues to be supported by the Department of Health.
BUT
- If it is to survive and make a real impact we need the Department of Health to prioritise promoting it and publicise its existence and to do so soon.
- We need to understand which organisations are involved – so that we can support them, lobby them and hold them to account.
- Despite his commendable support it would help the development and sustainability of Inclusion Health if it was clear that it was supported by a wide range of organisations outside government and not just by Steve Field and the Department of Health. This is because the NHS Future Forum is increasingly perceived as providing “cover for the governments efforts to privatise the NHS”.
What do you think?
The New Public Health – Emerging Practical Ideas
Solutions for Public Health published an important document just before Christmas. Co-Production for Health: A new model for a radically new world (National Colloquium) helps us keep our eye on the longer term ambition we will need if we are to use the opportunity created by the transfer of public health from the NHS to local government to modernise our approach to public health and health inequalities.
The document has credibility for three reasons:
First, it comes from a number of key organisations who are tasked with improving public health on the ground – the Chartered Institute for Environmental Health; Association of Directors of Public Health; the NHS Alliance; and the Association of Directors of Adult Social Services.
Second, it reminds us of what the big issues are:
- health Inequalities are widening and the gradient needs to be addressed.
- Its important to have a system that delivers the Marmot recommendations
- the impact of the recession and its implications for practice – resilience of communities in particular.
Third, it sets out 9 priority areas to focus on. Some are pretty obvious and should be familiar to leaders in any partnership or set of organisations working in complex systems such as the need for:
- Focussed agreed priorities which have meaningful outcomes for partners
- Delivery mechanisms in place to implement HWB decisions
- New funding mechanisms to drive change – don’t spend money on what does not work – decision makers need advice on how to proceed when evidence is strong and weak.
Others are more insightful, strategic and creative and start to carve out the basis for a new more inclusive approach to public health. These include:
- Intelligence – Using it intelligently – “JSNAs currently do not always access the wealth of data available at a local level. JSNA of the future need to link with intelligence held for example, by the fire and police services as well as the whole range of local government departments inufficient use has also been made of qualitative intelligence held within neighbourhoods and communities”.
- Assets – Asset-based approach to communities – “use communities positively to understand and harness their assets and resource, particularly around personalisaiton of budgets. There is … much statutory bodies can learn from … the voluntary sector in securing effective local involvement.
- Local Politicians – Elected members must buy in – the model will fail without elected members. “the reforms present an opportunity to secure engagement of elected members in more productive ways and create new champions for health and well being. …. It is crucial to create relevant narriatives and understanding for members about how they can make a real difference to health and wellbeing.”
- Partnership – A new partnership and leadership model – “the traditional model of the DPH as the sole advocate and champion for health must be consigned to the past” “We need a new conceptual model with the DPH working corporately alongside their colleagues in the local authority”
- Practical – Decisions for the future need to be practically based. The Public Health Workforce hs to change – “placing NHS public health teams within local government is not ‘click and drag’. Local Commissioners need pragmatic solutions based on the best evidence available – they need to know the implications and impact of different commissioning decisions.
- Capacity – Public Health Capacity on an industrial scale. “Achieving public health outcomes cannot rest with a relatively small specialist and practitioner public health workforce”
So the colloquium report starts to offer us a modernised view of public health that might be like this:
- More local
- Has a more inclusive view of public health capacity
- Puts a greater emphasis on partnership skills and on offering practical advice to commissioners
- Expects a more sophisticated view of intelligence
- Requires a re-balancing of the relationship with communities and citizens
What do you think?
David Nicholson in charge at the Department of Health!
 At the bottom right of the Department of Health website is a tag cloud which is an aggregation of terms that have been highlighted in Department of Health publications. Behind it is a popular tags list – which gives a numerical value to the tag cloud terms.
At the bottom right of the Department of Health website is a tag cloud which is an aggregation of terms that have been highlighted in Department of Health publications. Behind it is a popular tags list – which gives a numerical value to the tag cloud terms.
During the last three months of last year I have kept an (almost) weekly check on the tag list. The figures are not completely exact – I did miss a couple of weeks – however the overall shape of the data holds true. You will note that I have just added up the total number of tags for the whole of the survey period – they are not weekly averages.
First –all the tag cloud data is here – you can see all the tags used – I have tried to group these into categories that make sense – you may disagree with some of the groupings – more of these later.
Here are some findings.
Leaders voice
David Nicholson is clearly the guvnor! If you were expecting two of the most senior Department of Health Officials – the Chief Medical Officer – Sally Davies or the Permanent Secretary – Una O’Brien to feature strongly then you will be disappointed – there is no mention of either of them.
In fairness to Nicholson – until the current government the Department of Health has by and large been the Department of the NHS so we should expect him to feature prominently. However as reform plays out one would think there would be an increasing dissonance between such displays of centralist leadership vested in one person and the ambition for greater decentralisation.
Its also interesting that there is no mention of Andrew Lansley or any of his ministerial chums. I assume that this is DH policy. Mind you given the deeply unpopular NHS reforms this is probably a wise move.
Priority Areas
Here are the 15 most popular tags used by DH during October to December 2011
Comment
- Given the time of year the appearance of flu at the top of the list is no suprise. Again, its interesting to note that David Nicholson is the second most used tag on the whole DH Web Site!
- Adult Social Care features once – coming in at 9th.
- Public Health comes in at 14th with ‘diet’.
DH Priorities overall.
This final graph shows all the data grouped into the categories I mentioned at the start of the article.
Comment
- I know that is not suprising to see that DH activity is dominated by the day to day management of the NHS – however the sheer scale of this stands out in the graph above – a fixation with the NHS – rather than with health and wellbeing.
- System reform is the next most popular tag after NHS management.
- Local Government merits little focus – as does adult social care
- There are no tags referencing – the voluntary sector, health inequalities, inclusion health – which gives an indication of how importantly DH takes these issues.
Conclusion
If the Government Health Reforms are implemented how might the shape of this graph look in 18 months time?
- No NHS management tags?
- Nothing on system reform?
- A greater focus on local government delivery?
- More on Adult Social Care?
- … and of course no mention of David Nicholson!
What do you think?
Keeping an eye on the NHS Commissioning Board
The new Chair of the NHS Commissioning Board – Malcolm Grant Provost of University College London – is not unused to conflict. He has been attacked by the right and the left in recent times.
Now that he has taken responsibility for the governance of the NHS CB- worth at least £90bn of our money – we need to quickly try to understand him.
Aside from the Government supporters of Grant include Aaron Porter – ex NUS President who fell from grace over his failure to organise assertive opposition to the student fee increases and Richard Horton Editor in Chief of the Lancet who defends his independence of mind and ability to drive through major change.
Critics on the left point out his poor record to inequalities. When he was challenged to introduce the London Living Wage for some of the lowest paid staff (cleaners) at University College London where he is the Provost he initially refused saying that to do so was a luxury that the university could not afford. It was only after a successful campaign by unions, students and the press that he did a U turn and agreed to do it – although a year later this has still to be fully implemented.
He earns in the region of £400,000 a year.
Earlier this month a general meeting of the University of London Student Union voted ‘no confidence’ in his leadership – in part this was in response to his perceived championing of outsourcing of public services and his willingness to fine and take student activists to court as well as his track record on low wages.
Health Select Committee
Its worth reading the pre-appointment hearing held by the health select committee held on the 18th of October 2011 which Grant attended. There is a lot in there – but one of weaker areas were his responses to how the NHSCB would be held to account.
As Rosie Cooper MP states (Q53) in response to an answer from Malcolm Grant:
“You will be accountable to the people via the press but not via structures. It is unbelievable”.
In his detailed answers to many questions I remain unclear how he believes the NHSCB will fulfil its independent role – and question and publicly challenge government policies if they feel that these are to the detriment of population health and wellbeing. For example he would not be drawn on commenting on cuts to Public Health Observatories (Q67).
Finally he describes the health and social care bill as ‘unintelligible’ and says that ‘he is not a patient of the NHS’.
So a mixed bag – he is clearly tough and used to conflict; willing to take unpopular positions and weak on accountability to the public……….and prefers to get his health care from the private sector.
Accountability in practice
2 months after the select committee we have the first ‘public’ meeting of NHS Commissioning Board – held on the 9th December. There is a rather poor quality video of the first 12 minutes or so. From this we can deduce that this public meeting (There is some confusion as to whether this was a public meeting (website) or one held in public (Malcolm Grant) either way the public bit lasted just over 12 minutes – then the video ends abruptly.
This meeting was held in a video conference room in Quarry House – attended by 9 people (one of whom was joined virtually by video link)
They are not introduced – so I have no idea who most (9 white people, 7 men and 2 women – one of whom appears to be taking minutes) are. Aside from Bruce Keogh, Malcolm Grant and David Nicholson.
Some of the messages from Malcolm Grant were:
- Partnership working – CCGs, Patient Groups, Local Authorities the HEA and PHE
- Recognition of public support for NHS – almost doubled over the last 10 years.
- Need for greater attention to the public health agenda
At the time of writing the minutes of the meeting are not up yet. The next Public Meeting is scheduled for the 2nd of February 2012 and notice of it will appear 5 days before here.
At the earlier Select Committee he stated that he hoped his 5 non exec directors would be appointed by January 2012 – so we should expect to see them at this meeting.
So where does this leave us?
First, if you are a low paid manual worker in the NHS – I would not expect much sympathy from him.
Second, it feels a bit like the Italian experience – we seem to have a significant part of publicly funded service under the control of technocrats – with no clear accountability back to the public for their actions.
Third, the mechanisms that they have in place to communicate and involve feel….. amateurish. Who fancies going to the next ‘public’ meeting in February?